Evidence indicates that ankle fractures are becoming increasingly more common among older people, presenting a significant burden to the US healthcare system, with annual costs exceeding $17 billion for osteoporosis-related fractures, explains Eric So, DPM. “The injury pattern can be quite complex due to the poor bone quality—a proven risk factor for surgical failure and postoperative complications—and strength,” he says. “Assessing bone mineral density in elderly patients who suffer ankle fractures can be an important consideration in the perioperative management of an ankle fracture.”
Comparing BMD
With inconsistent findings from prior research regarding the relationship between ankle fractures and osteoporosis, Dr. So and colleagues conducted a systematic review and met-analysis of observational, cross-sectional studies of high methodological quality in order to quantify the relationship between BMD in elderly patients with ankle fractures compared with that of cohorts without ankle fractures. In the final meta-analysis, seven studies were included that measured BMD using dual-energy X-ray absorptiometry. In all seven, postmenopausal women, women older than 50, or patients with a history of fragility fracture of the ankle were compared with a control group of women older than 50 or healthy postmenopausal women without a history of fragility ankle fractures. Among more than 25,000 patients, the average age was approximately 65.
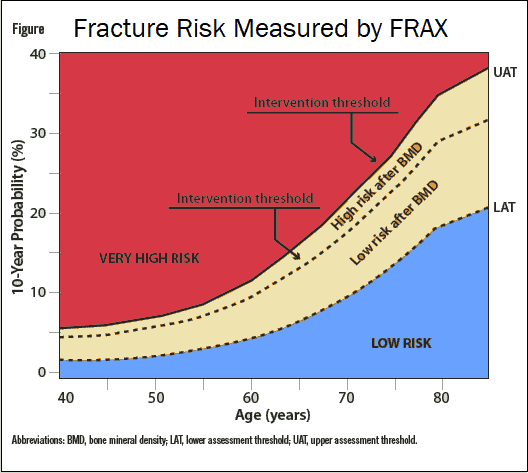 Results of the meta-analysis indicate that patients with ankle fractures had a reduced BMD when compared with health controls of similar age, with an effect size of 0.34 (Figure). Whereas BMD measurements of the lumbar spine, total hip, distal one-third radius were not associated with ankle fractures, an association was determined between low BMD at the femoral neck and ankle fracture in the studied patients. “It should be noted that this study does not establish a causal relationship, but rather an association,” adds Dr. So. “However, this relationship should be studied further. Clinicians with a strong interest in osteoporosis should be aware that elderly patients with ankle fractures may benefit from bone density screening.” He notes, however, the variability in association with ankle fractures depending on the anatomic site.
Results of the meta-analysis indicate that patients with ankle fractures had a reduced BMD when compared with health controls of similar age, with an effect size of 0.34 (Figure). Whereas BMD measurements of the lumbar spine, total hip, distal one-third radius were not associated with ankle fractures, an association was determined between low BMD at the femoral neck and ankle fracture in the studied patients. “It should be noted that this study does not establish a causal relationship, but rather an association,” adds Dr. So. “However, this relationship should be studied further. Clinicians with a strong interest in osteoporosis should be aware that elderly patients with ankle fractures may benefit from bone density screening.” He notes, however, the variability in association with ankle fractures depending on the anatomic site.
A Screening Process for Undiagnosed Osteoporosis?
“The presence of an ankle fracture in the elderly could be an indicator of potential bone fragility similar to other typical fragility fractures,” Dr. So explains. “Its occurrence is a clinical opportunity to assess fracture risk in the elderly population. The implications from our study form the basis to perform further testing, which may prevent subsequent secondary fractures. Currently, fracture liaison services typically do not include ankle fractures as a clinical event that would warrant further bone density testing. Our results could be used to assign the appropriate subgroup of patients with ankle fracture to treat the ankle fracture, assess future fracture risks, and serve as a stimulus for secondary fracture prevention by limiting gaps in anti-osteoporosis initiation. In essence, this data can used to help form the basis for a screening process for undiagnosed osteoporosis, akin to current clinical screening guidelines for colonoscopies or mammograms.”
Dr. So notes that this research was the first to quantify the relationship between ankle fractures among elderly patients and BMD, and that while a mild association was seen with a low femoral neck bone density, further research is required. “Future investigations should be focused on determining the percentage of elderly ankle fracture patients with undiagnosed osteoporosis by obtaining bone density at the time of ankle fracture occurrence,” he says. “Other investigations should focus on assessing fracture risk and analyzing the cost effectiveness of osteoporosis screening for ankle fractures in elderly patients.”


 Rebecca Shover
Rebecca Shover