Pediatric surgery trainees must have 2 more years of experience beyond what the American Board of Surgery (ABS) requires for general surgery trainees. This additional training enables them to work with cases that are specific to the field of pediatric surgery so that they can master operations for complex medical conditions. “Knowledge and experience in specific index pediatric surgery cases is essential to ensuring competency,” says Fizan Abdullah, MD, PhD. He adds that specific case volume has been used as a benchmark to help ensure experience for both general and pediatric surgery trainees.
In 2012, the Association of Program Directors in Pediatric Surgery and the Residency Review Committee approved a list of minimum case numbers in 18 key operative categories for all pediatric surgery trainees. This list was also endorsed by the Pediatric Surgery component board of the ABS.
Despite these guidelines, however, there are still barriers surrounding the provision of adequate experience for pediatric surgery trainees, with an increasing number of trainees and a relatively fixed number of rare disease cases available for training. In addition, the number of practicing pediatric surgeons has also increased rapidly in the last 40 years, but again, the number of rare cases is fixed here too. This means that pediatric surgeons generally see fewer rare and complex cases in their practices, which could potentially decrease competency. This is important considering there has been increased scrutiny on surgeon competency and patient safety.
New Data
Recently, Dr. Abdullah and colleagues published a study in JAMA Surgery that described the experiences of practicing pediatric surgeons by reviewing case log data that were submitted to the ABS during the recertification process. “Our goal was to determine what type of operative experience pediatric surgeons were reporting in their practice,” Dr. Abdullah says. The retrospective review examined 5 years of pediatric surgery certification renewal applications from 308 surgeons, which were submitted to the Pediatric Surgery Board from 2009 through 2013. Surgeons were categorized according to recertification at 10, 20, or 30 years.
According to the results, on average each surgeon preformed 433 pediatric surgical procedures, but few were in the complex and rare category. Appendectomy was the most commonly performed procedure, followed by non-operative trauma management and inguinal hernia repair for children younger than 6 months of age. After categorizing the findings by organ system, the majority of procedures performed per year were abdominal in nature, followed by hernia repair and cardiovascular procedures (Table below).
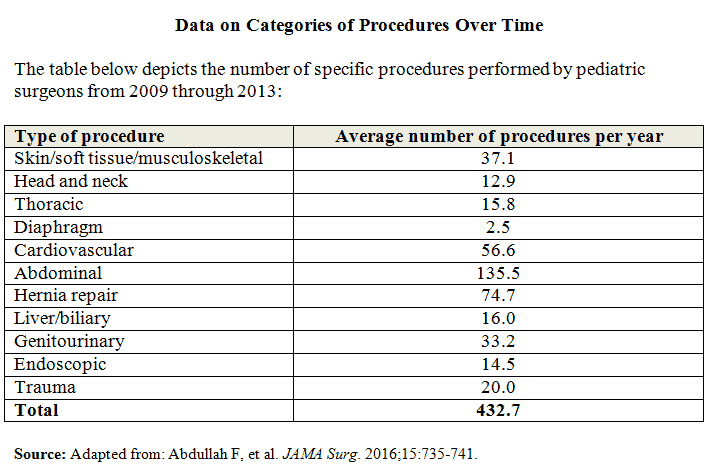
Dr. Abdullah says the findings indicate that practicing pediatric surgeons appear to receive limited exposure to index cases after training, a result that raises questions regarding the maintenance of competency. “Our results showed that pediatric surgeons performed an average of fewer than two procedures per year in operations that were classified as rare pediatric surgeries,” he says. Furthermore, in terms of specific procedures, only about one-third of surgeons had performed a neuroblastoma resection while a little more than half performed a kidney tumor resection. Only about 40% performed an operation to treat biliary atresia or a choledochal cyst in the preceding year.
Laparoscopy was more frequently performed in the 10-year recertification group for Nissen fundoplication, appendectomy, splenectomy, gastrostomy/jejunostomy, orchidopexy, and cholecystectomy but not for lung resection. Laparoscopy was used more frequently by surgeons recertifying in the 10-year group than by surgeons recertifying in the 20-year or 30-year groups.
Important Implications
“One way to augment the low number of operative index cases is to increase the use of simulation-based education for practicing pediatric surgeons,” Dr. Abdullah says. “As we move into the future, this and other modular approaches that provide the opportunity for skill refinement may be especially important tools for practicing pediatric surgeons as well as trainees.” For instance, since some surgeons who were trained before the emergence of laparoscopy remain cautious in introducing minimally invasive surgery to their practice, additional simulation-based training could help build competency in this area.
Another option to consider is further subspecializing pediatric surgeons, a phenomenon that is already occurring on some level at larger children’s centers. This can help address the issues of technical competency and will help facilitate the more-frequent performance of operations for rare cases.
Dr. Abdullah says that the results of this study are particularly important as the pediatric surgery community grapples with issues surrounding the maintenance of competency in performing complex cases because they are performed infrequently. “Our findings highlight the importance of increasing educational efforts for pediatric surgeons to help prevent the erosion of competency,” he says.
Fizan Abdullah, MD, PhD, has indicated to Physician’s Weekly that he has or has had no financial interests to report.


 PhysWeekly
PhysWeekly