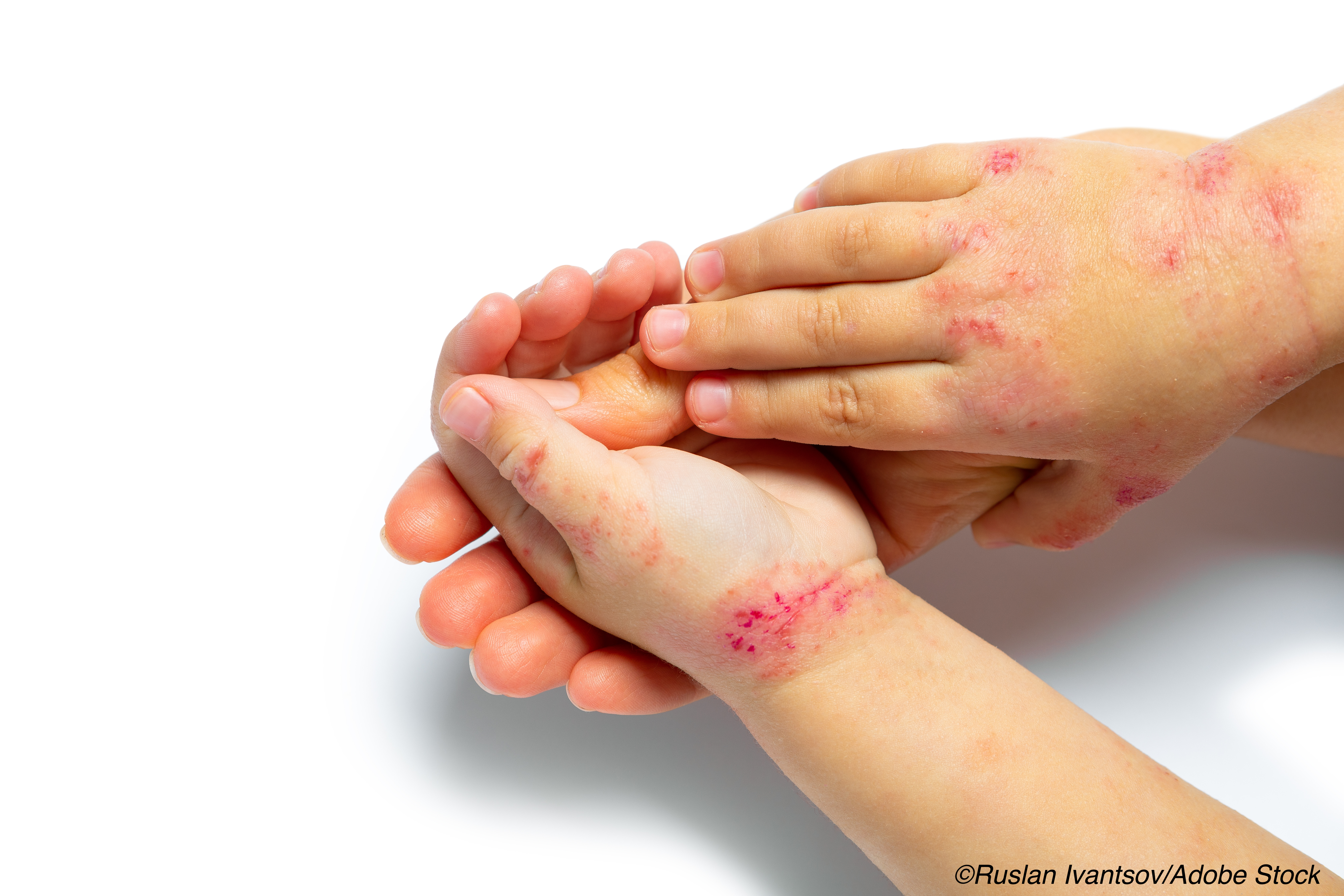
Two newly published studies suggested a link between childhood eczema and poorer educational achievement, with one study finding more learning disabilities, and another, lower secondary school attainment in children with a diagnosis of atopic dermatitis.
Having eczema was associated with a 50% greater likelihood of not completing lower secondary education equivalent to junior high graduation in a population-based cohort study from Denmark, and a 16% increased risk of not completing high school.
And a cross-sectional study of data from the Pediatric Eczema Elective Registry (PEER) in the United States found a three-fold greater risk for learning disabilities among children with severe or very severe eczema, compared to those with clear or almost clear skin.
Both studies were published online April 14 in JAMA Dermatology.
In accompanying commentary, dermatologist Katrina Abuabara, MD, of the University of California, San Francisco, wrote that while many questions remain unanswered, the latest findings do suggest “an association among atopic dermatitis (AD), learning, and education.”
Abuabara noted that in both studies, the observed associations were independent of other atopic diseases, including asthma and rhinitis, and other neuropsychiatric conditions.
“This observation suggests that screening children with AD may be a good way to identify those who may benefit from educational interventions, but more work is needed,” she wrote.
Atopic dermatitis affects roughly one in five children in Western countries, and the condition has been linked to poorer sleep, attention, and memory due to itching.
Given that all of these things could impact academic performance, researcher Sigrun Alba Johannesdottir Schmidt, PhD, of Denmark’s Aahus University Hospital, and colleagues, used routinely collected health data from Denmark to explore whether children with hospital-diagnosed AD have an increased risk for failing to advance academically.
The study included 61,153 children, including 5,927 with a diagnosis of AD (56.4% male) before their 13th birthday and 55,226 from the general population (56.5% male) born in Denmark up until mid-1987.
In an effort to account for familial factors, a secondary analysis included exposure-discordant full siblings of children with eczema as a comparison cohort.
Among the main study findings:
- Compared with matched children from the general population, children with AD were at increased risk for not attaining lower secondary education (2.5% vs 1.7%; adjusted RR, 1.50; 95% CI, 1.26-1.78) and upper secondary education (19.8% vs 16.4%; RR, 1.16; 95% CI, 1.09-1.24), but not higher education (51.9% vs 53.1%; RR, 0.95; 95% CI, 0.91-1.00).
- The absolute differences in probability were less than 3.5%.
- The comparison of 3,259 children with AD and 4,046 of their full siblings yielded estimates that were less pronounced than those in the main analysis (adjusted RR for lower secondary education, 1.29 [95% CI, 0.92-1.82]; adjusted RR for upper secondary education, 1.05 [95% CI, 0.93-1.18]; adjusted RR for higher education, 0.94 [95% CI, 0.87-1.02]).
The researchers noted that the tendency for eczema to improve with age may explain the observed decline in risk with increasing educational level.
“Our study supports the findings of previous studies, and the unique sibling design addresses concerns about confounding by familial factors,” Schmidt et al wrote.
In the cross-sectional study from the U.S., researcher Joy Wan, MD, of the University of Pennsylvania Perelman School of Medicine, Philadelphia, and colleagues used PEER data from late 2004 through November 2019 to compare the prevalence of learning disability in children with AD to those without the skin disorder.
AD severity was measured using the Patient Oriented Eczema Measure (POEM) score, which ranges from 0 to 28 (0-2, clear or almost clear skin; 3-7, mild; 8-16, moderate; 17-24, severe; and 25-28, very severe).
Among the 2,074 participants with AD (53.8% female; median [interquartile range (IQR)] age, 16.1 [13.9-19.5] years at 10-year follow-up), 169 (8.2%) reported a diagnosis of a learning disability.
Children with a learning disability versus those without a learning disability were more likely to have worse AD severity, as measured by the median POEM score (5 [1-10] vs 2 [0-6]; P<0.001), POEM severity category (moderate AD: 29.8% vs 17.0%; severe to very severe AD: 8.9% vs 4.5%; P<0.001); and self-report (moderate AD: 29.2% vs 20.7%; severe AD: 6.5% vs 3.4%; P<0.001).
Upon multivariable logistic regression modelling adjusted for sex, age, race/ethnicity, annual household income, age of AD onset, family history of AD, and co-morbid conditions, Wan and colleagues found that children with mild AD (odds ratio [OR], 1.72; 95% CI, 1.11-2.67), moderate AD (OR, 2.09; 95% CI, 1.32-3.30), and severe to very severe AD (OR, 3.10; 95% CI, 1.55-6.19) on the POEM were significantly more likely to have reported a learning disability than those with clear or almost clear skin.
In her commentary, Abuabara noted that the recognition of a possible link between AD and learning issues represents “a new chapter in our understanding of AD, but currently there are more questions than answers.”
“As dermatologists, we may empathize with the social implications of patients’ health conditions, but we may also feel limited by the tools available to address these challenges. Social aspects of the patient experience are often overlooked in research. A focus on outcomes beyond the skin, interdisciplinary collaborations, and the inclusion of patients and caregivers in research can help us to better understand and treat the whole patient,” she concluded.
-
Newly published research suggested a link between childhood eczema and poorer educational achievement.
-
Having eczema was associated with a 50% greater likelihood of not completing lower secondary education equivalent to junior high graduation in a population-based cohort study from Denmark, and a 16% increased risk of not completing high school.
Salynn Boyles, Contributing Writer, BreakingMED™
Funding for the study by Johannesdottir Schmidt et al was provided by the Aase and Ejnar Danielsens Fund and others. Researcher Mette Deleuran reported receiving fees for various services from LEO Pharma A/S, AbbVie Inc, Lilly, Novartis AG, Pfizer Ince, Regeneron Pharmaceuticals, and Sanofi.
Funding for the study by Wan et al was provided by the Dermatology Foundation and Bausch Health. Dr. Wan reported receiving grants from the Dermatology Foundation during the conduct of the study and grants from Pfizer outside the submitted work.
Commentary writer Katrina Abuabara reported receiving personal fees from TARGET Real World Evidence and research grants from Pfizer.
Cat ID: 105
Topic ID: 75,105,730,105,449,138,192,923,925


