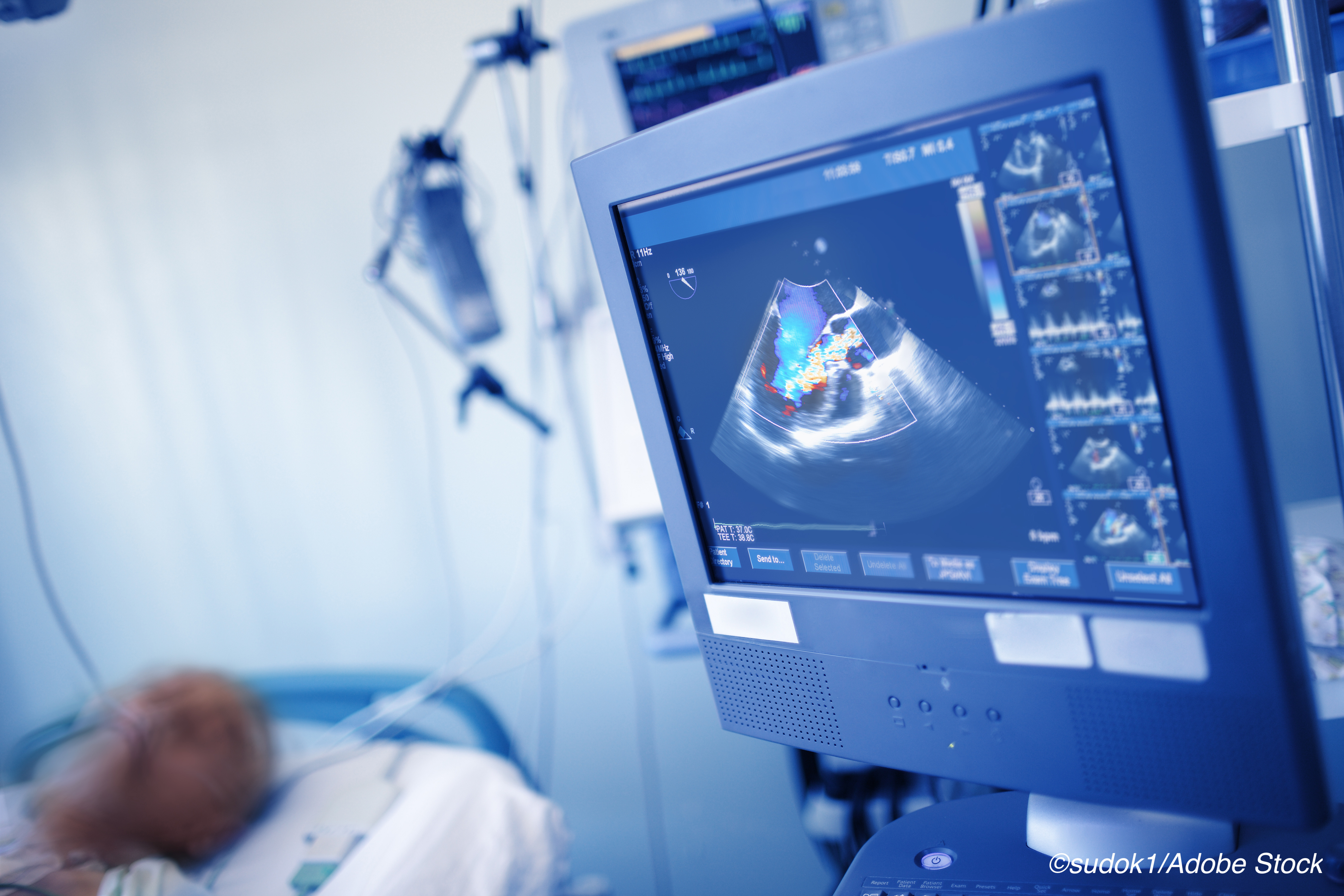
Nearly two-thirds of Covid-19 patients who underwent echocardiography had heart abnormalities that put them at an increased risk for in-hospital death, researchers reported.
In a registry-based study, and in 305 patients with lab-confirmed SARS-CoV-2 infection who had transthoracic echocardiography (TTE) and ECG evaluation, 62.6% had biomarker evidence of myocardial injury, according to Gennaro Giustino, MD, of Icahn School of Medicine at Mount Sinai in New York City, and co-authors.
The majority (n=118/190) had myocardial injury at the time of hospital admission, while the rest developed myocardial injury during the hospitalization, the authors added. TTE was indicated mostly for chest pain, shortness of breath, and/or cardiac troponin T (ctN) elevations, they wrote in the Journal of the American College of Cardiology.
Guistino and co-authors found that rates of in-hospital mortality varied according to the presence of myocardial injury and TTE abnormalities. Specifically, the rate was 5.2% in patients without myocardial injury, with or without TTE abnormalities; 21.0% in those with myocardial injury but without TTE abnormalities; and 31.2% in those with myocardial injury and TTE abnormalities.
Myocardial injury with TTE abnormalities was tied to a higher risk of death following multivariable adjustment for other complications of Covid (adjusted OR 3.87, 95% CI 1.27 to 11.80), the authors determined, while myocardial injury without TTE abnormalities did not carry the same mortality risk after adjustment (adjusted OR 1.00, 95% CI 0.27 to 3.71).
Additionally, Covid patients with myocardial injury had more ECG abnormalities and higher levels of inflammatory and coagulation biomarkers, as well as any major echocardiographic abnormalities versus patients without myocardial injury (63.2% vs 21.7%, odds ratio 6.17, 95% CI 3.62-10.51).
TTE abnormalities included global left ventricular dysfunction (LV), regional wall motion abnormalities, diastolic dysfunction, right ventricular dysfunction, and pericardial effusions, they noted.
Giustino’s group concluded that “TTE in patients with troponin-positive Covid-19 syndromes provides useful prognostic information. The association between myocardial injury and mortality (especially in those with echocardiographic abnormalities) is likely multifactorial and possibly both correlative and causative in nature.”
In an editorial accompanying the study, Carl Lavie, MD, of John Ochsner Heart and Vascular Institute in New Orleans, and co-authors endorsed “routine serial measurement of these biomarkers in patients hospitalized for Covid-19 with TTE…this study provides very practical evidence to improve current clinical practice during this and possibly other such pandemics.” One of the co-authors is Giuseppe Lippi, MD, of the University of Verona in Italy, who was an author on the above-mentioned meta-analysis.
Lavie’s group explained that the ACC currently recommends that Covid-19 patients with suspected acute myocardial infarction undergo cTN troponin measurement. But they suggested that the ACC guidance “seems somehow inadequate,” as the current findings offer “evidence that cTn-positive Covid-19 patients may benefit from routine TTE, which would allow practitioners to garner useful prognostic information and to establish specific therapeutic options in patients with cardiac injury.”
Lavie and co-authors argued that ACC criteria for cTn measurement should be expanded to all patients infected with SARS-CoV-2 — and not just those with a clinical suspicion of cardiac ischemia – while Giustino’s group recommended that “in the appropriate clinical scenario, TTE (or a point-of-care ultrasound) may be considered among patients with Covid-19 infection and biomarker evidence of myocardial injury to potentially identify those who might benefit from expedited invasive management.”
However, the retrospective study was limited by a small sample size, no cardiac MRI data, and a reliance on “manual electronic health record extraction from multiple institutions,” the authors explained.
Giustino and co-authors evaluated data from the Cardiac Injury Research in Covid-19 registry (CIRC-19) that includes seven clinical in New York City and Milan. Patients had a mean age 63 years; 67.2% men, the majority were white, and over half had hypertension.
Patients also had a median BMI of 28 kg/m2, which Lavie’s group said was noteworthy as patients with obesity “tend to experience worse outcomes and more critical illness in Covid-19 and are known to have more cardiac structural and functional abnormalities on TTE or other cardiac imaging, as well as more comorbidities associated with worse outcomes.”
The authors reported that older patients and those with hypertension or chronic kidney disease were more likely to experience myocardial injury. Patients with myocardial injury also had greater LV volumes, wall thickness, and left atrial volumes, although most had preserved LV function.
The time to TTE from hospital admission was a median of 4 days for each patient, according to the authors. ICU admission was necessary in 43.9% of the cases while 34.5% required mechanical ventilation.
In terms of cardiac catheterization, the authors reported that only 3.6% of the patients required the procedure, and over 72% of those had acute coronary syndrome (ACS). “Patients with confirmed ACS compared with other causes of troponin elevation had a different clinical profile from patients with other causes of myocardial injury, including more frequent chest pain at the time of clinical presentation, more ECG changes, lower levels of inflammatory biomarkers, and all had regional wall motion abnormalities on TTE,” they wrote.
- Cardiac structural abnormalities were present in nearly two-thirds of patients with myocardial injury and Covid-19 who underwent transthoracic echocardiography (TTE).
- Myocardial injury was linked with increased in-hospital mortality, particularly if TTE abnormalities were present.
Shalmali Pal, Contributing Writer, BreakingMED™
The study was supported by Regione Lombardia Welfare.
Giustino disclosed relevant relationships with Bristol Myers Squibb and Pfizer.
Lavie and co-authors disclosed no relevant relationships with industry.
Cat ID: 5
Topic ID: 74,5,5,914,190,926,192,927,925,934


