It’s jarring every time. The sudden crash in patients with COVID-19
All over the world, seemingly mild cases of COVID-19 rapidly morph into severe cases that involve the lower lungs. This may be attributed to “the cytokine storm.” There are many variations on this phenomenon, and they go by many names: systemic inflammatory response syndrome, cytokine release syndrome, macrophage activation syndrome, hemophagocytic lymphohistiocytosis.
A cytokine storm is an overproduction of immune cells and their activating compounds—cytokines—which, in something like a flu infection, is often associated with a surge of activated immune cells into the lungs. The resulting lung inflammation and fluid buildup can lead to respiratory distress and can be contaminated by a secondary bacterial pneumonia. This increases the risk of mortality in patients.
It’s not the most widely-understood phenomenon, but it occurs in several types of infections and autoimmune conditions. It appears to be particularly relevant in outbreaks of new flu variants. Cytokine storm is now seen as a likely major cause of mortality in the 1918-20 “Spanish flu”–which killed more than 50 million people worldwide and the H1N1 “swine flu” and H5N1 “bird flu” of recent years—and now COVID-19. In these epidemics/pandemics, sometimes patients at higher risk to die were often relatively young adults with seemingly strong immune reactions to the infection.
The surge in immune molecules can result in the fatal shutdown of multiple organs.
In an interview with UAB News last month, Randy Cron, MD, an expert on cytokine storms at the University of Alabama at Birmingham, explains how cytokine storm syndrome may be at work in the current COVID-19 pandemic and how it can be detected and possibly treated. Here is an excerpt:
What host reaction do you think may be a cause of death in COVID-19 cases?
Dr. Cron: “From reading the literature primarily out of China, many of the severely ill coronavirus-infected patients appear to have clinical and laboratory features of a cytokine storm syndrome, or CSS, which is frequently fatal.”
Are there treatments for CSS?
Dr. Cron: “Although we don’t know what specifically will benefit CSS associated with COVID-19, we have experience with treatments for other CSS cases. While we are attempting to develop vaccines for COVID-19 and are trialing novel or re-purposed anti-iral therapies for COVID-19, let us also not forget to treat the patient with all we have to offer to help save lives. We need to address the immediate needs for the significant numbers of patients becoming critically ill in the current pandemic. As rheumatologists, we have much to offer on the front lines of helping to recognize and treat these critically ill individuals with complications of hyper-inflammation.”
Read the full interview at UAB News.
How to Spot It
An elevated serum ferritin test—which is cheap, readily available and quick—is a good first step for screening for CSS. There are a variety of other tests that can then help confirm or deny the presence of a cytokine storm syndrome.
According to Dr. Cron, a patient battling a cytokine storm may have an abnormally fast heart rate, fever and a drop in blood pressure. Apart from a surge in interleukin-6, the body may also show high swirling levels of molecules called interleukin-1, interferon-gamma, C-reactive protein and tumor necrosis factor-alpha.
Dr. Cron told the NY Times that if this storm develops, it becomes obvious a few days into the infection. A patient battling a cytokine storm may have an abnormally fast heart rate, fever and a drop in blood pressure. Apart from a surge in interleukin-6, the body may also show high swirling levels of molecules called interleukin-1, interferon-gamma, C-reactive protein and tumor necrosis factor-alpha.
The sooner doctors spot and treat the condition, the better the chance of survival. Surprisingly—or not surprisingly—there’s a simple, rapid test called an elevated serum ferritin test (among other tests), which is a good first step to detect if a person has been hit by a cytokine storm.
“Although we don’t know what specifically will benefit CSS associated with COVID-19, we have experience with treatments for other CSS cases,” Dr. Cron says in his UAB interview. “There are both broadly immunosuppressive approaches, such as high-dose corticosteroids, and more novel targeted approaches that go after inflammatory cytokine proteins. These include the interleukins IL-1 and IL-6, and interferon-gamma.”
Is there Recent Data on Cytokine Storms?
A recent pre-print study reviews the role of cytokines in SARS-CoV-2 infection.
Not all patients with COVID-19 develop the same symptoms, but the immunological determinants of a poor prognosis are unknown. In this pre-print article, Yang, Y et al. followed a cohort of 53 clinically moderate and severe patients; they conducted a multiplex screen for 48 cytokines and correlated these results with lab tests, clinical characteristics and viral loads. They found a marked increase of 14 cytokines in patients with COVID-19 compared with healthy controls.
Key Findings:
- Many elevated cytokines with COVID-19 onset compared to healthy controls (IFNy, IL-1Ra, IL-2Ra, IL-6, IL-10, IL-18, HGF, MCP-3, MIG, M-CSF, G-CSF, MIG-1a, and IP-10).
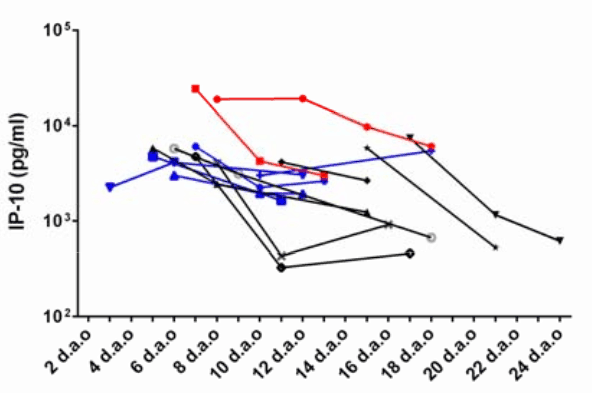
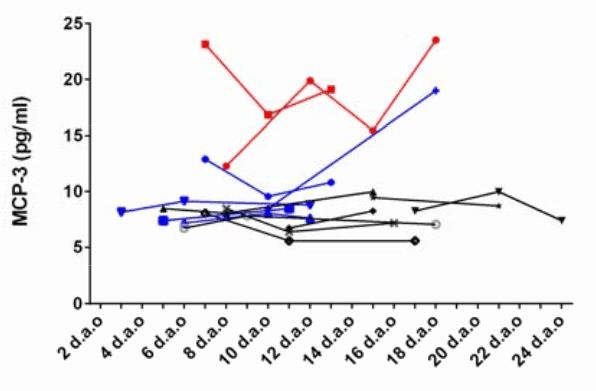
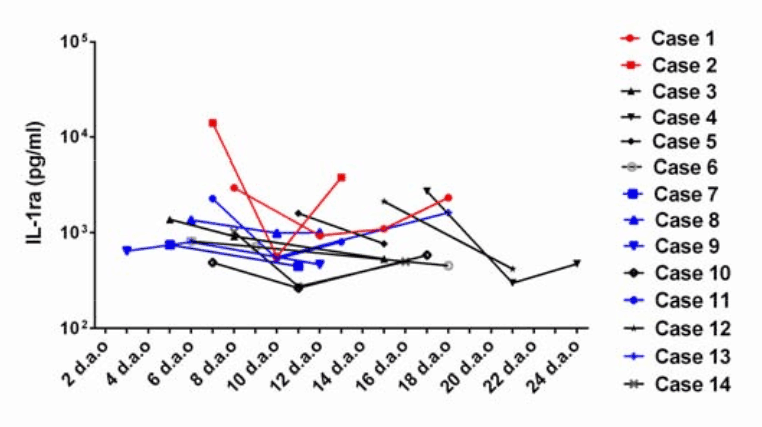
- IP-10, IL-1Ra, and MCP-3 (esp. together) were associated with disease severity and fatal outcome.
- IP-10 was correlated to patient viral load (r=0.3006, p=0.0075).
- IP-10, IL-1Ra, and MCP-3 were correlated to loss of lung function (PaO2/FaO2 (arterial/atmospheric O2) and Murray Score (lung injury) with MCP-3 being the most correlated (r=0.4104 p<0.0001 and r=0.5107 p<0.0001 respectively).
- Viral load (Lower Ct Value from qRT-PCR) was associated with upregulated IP-10 only (not IL-1Ra or MCP-3) and was mildly correlated with decreased lung function: PaO2/FaO2 (arterial/atmospheric O2) and Murray Score (lung injury).
- Lymphopenia (decreased CD4 and CD8 T cells) and increased neutrophil correlated w/ severe patients.
- Complications were associated with COVID severity (ARDS, hepatic insufficiency, renal insufficiency).
Importance: Outline of pathological time course (implicating innate immunity esp.) and identification key cytokines associated with disease severity and prognosis (+ comorbidities). Anti-IP-10 as a possible therapeutic intervention (ex: Eldelumab).
Figure: Dynamic changes of IP-10, MCP-10 and IL-1ra in severe cases of COVID-19 with different outcome and progression. The expression levels measured at the indicated time-points of 14 severe cases were shown. The fatal cases were marked in red. Cases in critical condition were marked in blue, and the others were cases with moderate disease or discharged at present
Source: doi: https://doi.org/10.1101/2020.03.02.20029975