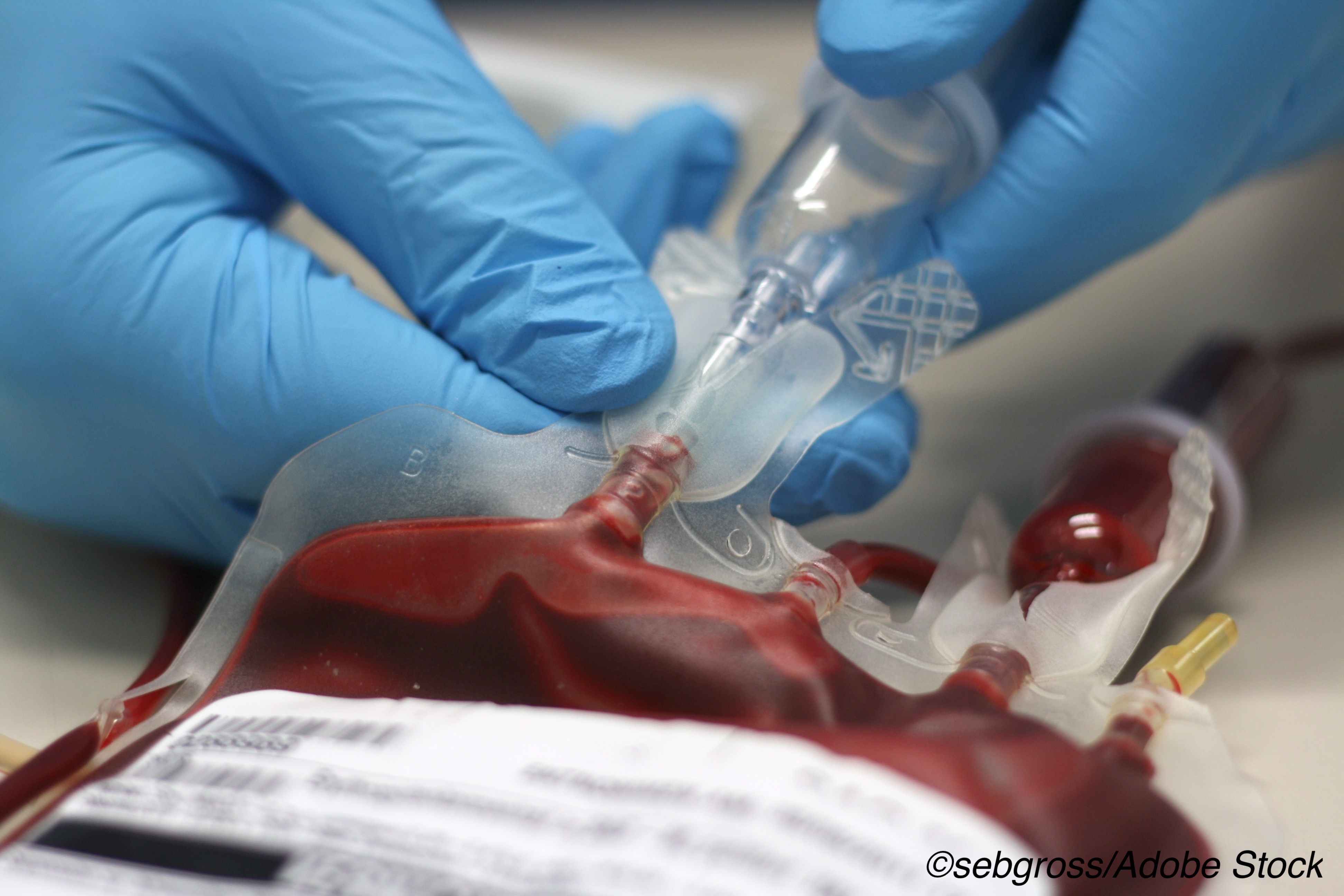
 Instead of treating patients with blood transfusions when their hemoglobin falls to 10 grams/dL — considered the liberal strategy — in the REALITY trial, the experimental groups was treated with transfusion when hemoglobin dropped to 8 g/dL, reported Gabriel Steg, MD, professor of medicine at Hopital Bichat/University of Paris.
Instead of treating patients with blood transfusions when their hemoglobin falls to 10 grams/dL — considered the liberal strategy — in the REALITY trial, the experimental groups was treated with transfusion when hemoglobin dropped to 8 g/dL, reported Gabriel Steg, MD, professor of medicine at Hopital Bichat/University of Paris.
Steg reported results of the 668-patient trial, which was a joint venture of researchers from France and Spain, during the final Hot Line session of the European Society of Cardiology’s annual meeting: ESC Congress 2020: The Digital Experience.
He explained that the study was initiated because of uncertainty over which of the strategies was best for patients in this category. About 5%-10% of patients with acute myocardial infarction also present with anemia; thus, clinicians are frequently faced with the question of whether or not to initiate blood transfusion. Evidence-based choices, unfortunately, are difficult to come by, since there is a paucity of studies and only mixed results among randomized trials of transfusion efficacy in the setting of AMI. For example, a pilot study by Cooper et al found that a liberal transfusion strategy might result in worse outcomes, but a pilot study by Carson et al found improved outcomes with a liberal strategy.
Of the 327 patients on the restrictive policy, 36 patients experienced the composite primary endpoint of cardiovascular events (11%), compared with 45 events (14%) of the patients who were treated more liberally, Steg said at a press conference.
That represented a 21% reduction in risk of those cardiovascular events and a 1.18 hazard ratio for treating with the liberal policy. Steg said that the pre-specified cut-off for non-inferiority was a 1.25 hazard ratio, so the restrictive strategy was statistically non-inferior to the liberal policy. He added that the study results could not be interpreted to suggest that the restrictive policy was superior to the liberal strategy – “but it was close.”
“Non-inferiority was confirmed in both the intention-to-treat and the on-protocol populations,” Steg reported in his oral presentation.
“When we looked at cost-effectiveness, we found that the restrictive policy was more effective and less costly – a rare combination that gives the strategy an 84% probability of being dominant,” Steg said. He said the cost benefit was driven by the reduction in use of blood products with the restrictive strategy.
The researchers also found that overall, there was no difference in adverse events in evaluating safety, although there were three infections that occurred in the liberal transfusion strategy and none in the more restrictive strategy, he said. There was also an increase in acute lung infections in the patients treated with the liberal strategy, the researchers reported. “Both those differences were statistically significant,” Steg said.
“These findings support the use of the restrictive strategy,” he said. “We didn’t see any downsides to this strategy. It is certainly non-inferior – bordering on superiority. There are only benefits in the side effects profiles, although we have to be careful because the number of events is small. On the blood management side, this is an extremely attractive strategy. Everything is going in the right direction.
“In my opinion, the only lingering question is whether the strategy is actually superior, and that is being addressed in another ongoing international trial being run by the National Institutes of Health in the United States,” he said.
“Blood is a precious resource, and transfusion is expensive, logistically cumbersome, and has some side effects,” Steg said. “The cost-effectiveness analysis indicated that the restrictive strategy had a high probability of being cost-saving while being outcome-improving.”
The joint French and Spanish study randomized patients to either group and defined the primary endpoint as the composite of death, non-fatal myocardial infarction, non-fatal stroke, or emergency revascularization prompted by ischemia. At discharge, patients in the restrictive group had a hemoglobin level of 9.7g/dL versus 11.1 g/dL in the liberal group. In the restrictive policy, blood transfusions were withheld until the 8 g/dL level was experienced, except in cases of excessive bleeding or if the patient was determined to be in shock. “Except for these individuals, we believe our findings are broadly applicable. Our enrollment into the study was brisk so we believe the patients were not over-selected and are quite representative of a broad patient population in myocardial infarction anemia,” they said.
Steg said 75% of the patients in the restrictive patient cohort were given transfusions compared with 86% of patients in the liberal strategy group. “The restrictive strategy saved 414 units of blood in the restrictive category compared with the liberal strategy,” he said.
The researchers also explored subgroups of patients in the study, but he said the results were fairly consistent, with no single group standing out in the analysis.
Marco Roffi, MD, director of interventional cardiology at University Hospital of Geneva, Switzerland, who served as discussant for the REALITY study, said, “I love the REALITY trial because it aims to provide a solution for a very important practical clinical dilemma — namely, whether or not you should transfuse anemic patient presenting with myocardial infarction.”
Roffi noted the lack of high quality data, and that guidelines do not give a formal recommendation.
“Actually, the primary outcome was positive,” he said, “meaning that the restrictive strategy was non-inferior to the more liberal one. The relative risk actually went in favor of the more restrictive strategy, albeit not reaching statistical significance for a superiority. So, what is the take home message from REALITY: In our opinion, it allows clinician to comfortably refrain from transfusing any patient presented with myocardial infarction, and this should lead to a reduction in the consumption of blood products.”
Roffi added that he believes guidelines should be changed from the current recommendation that a restrictive transfusion policy may be considered for hospitalized AMI patients to “a restrictive transfusion policy should be considered for hospitalized AMI patients.”
-
Note that the findings reported here are based on data presented at a medical conference that have not yet been published in a peer-reviewed journal.
-
Be aware that in this trial, use of a restrictive transfusion strategy was found to be both more clinically effective and more cost effective than a more liberal strategy.
Samuel Kailes, Contributing Writer, BreakingMED™
The study was funded by government agencies in France and Spain.
Steg disclosed relationships with Bayer, Merck, Servier, Sanofi, Amarin, Amgen, AstraZeneca, Boehringer-Ingelheim, BristolMyersSquibb, Idorsia, Mylan, NovoNordisk, Novartis, Pfizer, and Regeneron.
Roffi disclosed relevant relationships with GE Healthcare.
Cat ID: 204
Topic ID: 74,204,204,914,192,925,203


