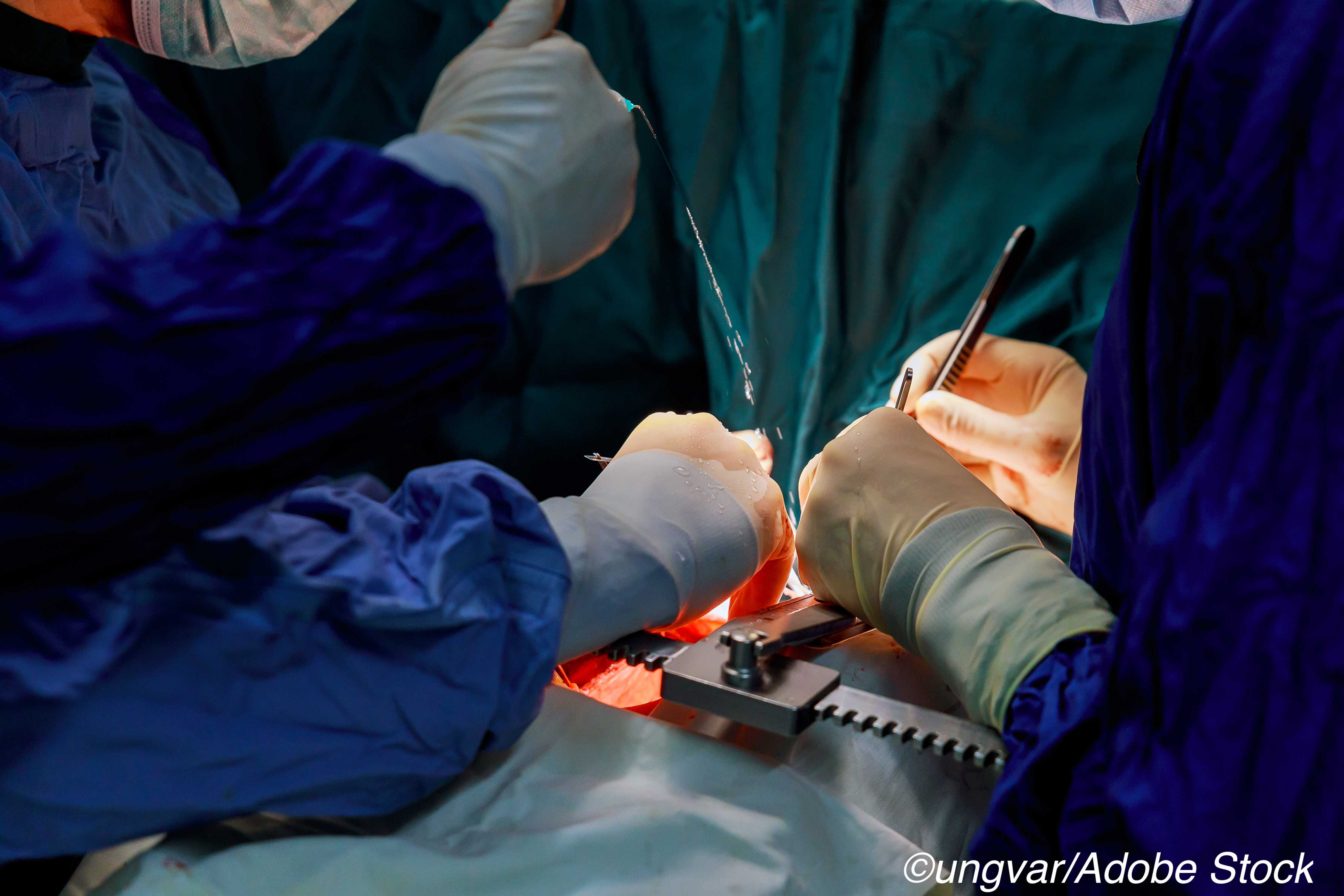
Mitral valve surgery success rates, as measured by successful valve repair and reduced mortality, were significantly better when procedures were performed at high-volume hospitals by more experienced surgeons in an analysis of U.S. clinical registry data.
Among patients undergoing valve surgery for severe primary degenerative mitral regurgitation (MR), increasing hospital and surgeon volumes were associated with lower risk-adjusted 30-day mortality, lower 30-day composite mortality and morbidity, and higher rates of successful repair in the study, which included more than 55,000 patients, treated at close to 1,200 hospitals.
The lowest versus highest hospital volume quartile had a higher 1-year risk-adjusted mortality (hazard ratio, 1.61, 95% CI, 1.31-1.98).
A significant, nonlinear association was also seen between surgeon mitral valve repair or replacement (MVRR) surgical volume and 30-day mortality, 30-day composite outcome and 30-day successful mitral valve repair in the study of data from the Society of Thoracic Surgeons’ Adult Cardiac Surgery Database, published July 1 in JAMA Cardiology.
“A significant hospital and surgeon volume-outcome association was identified for the primary outcome of operative mortality, as well as for the secondary outcome of composite in-hospital morbidity plus operative mortality, successful mitral valve repair of primary mitral regurgitation, and 1-year mortality, but not for 1-year mitral valve re-operation or hospitalization for heart failure,” wrote researcher Vinay Badhwar, MD, of West Virginia University, Morgantown, and colleagues.
They added that the study findings “may provide further support for efforts to regionalize mitral valve surgery” for primary mitral regurgitation, including for asymptomatic patients who meet guideline criteria for mitral valve repair or for patients seeking minimally-invasive- or robotic surgeries.
“Such cases may be better suited to experienced mitral valve surgeons and centers based on volume,” Badhwar and colleagues wrote.
Prior to the study’s publication, contemporary volume-outcome associations for mitral valve surgery had not been accessed at the national level. Likewise, the identification of “mitral reference centers” has not been backed by rigorous data, the researchers wrote.
“This important information has the potential to shape quality improvement, patient-physician referral patterns and resource allocation regarding the management of primary mitral regurgitation,” they wrote.
Their multicenter, cross-sectional, observational study included data from the Society of Thoracic Surgeons database on patients undergoing isolated MVRR for primary mitral regurgitation between mid-2o11 through 2016.
The analysis included 55,311 isolated mitral valve operations for primary mitral regurgitation performed during the period.
Annualized hospital volume of mitral valve surgery was analyzed both as a continuous variable and as a categorical variable in quartiles.
The median annual hospital MVRR volume among the 1,094 hospitals included in the analysis was 23 (patho, 11-46), and the median annual surgeon MVRR volume was 12 (IQR, 5-25). Quartiles were chosen to ensure an adequate number of hospitals in each volume category and to protect hospital identify.
In a comparison of the lowest versus highest quartiles with regard to procedure volume:
- Adjusted 30-day mortality after isolated MVRR for primary mitral regurgitation was greater in the lowest hospital volume quartile (1.36%; 95% CI, 1.12%-1.66%), compared with the highest hospital volume quartile (0.72%; 95% CI, 0.61%-0.84% (adjusted OR, 2.06; 95% CI, 1.47-2.90).
- At 1-year follow-up, the lowest hospital-volume quartile had increased risk adjusted mortality (9.58%; 95% CI, 7.86%-11.27%) compared with the highest volume quartile (6.20%; 95% CI, 5.82%- 6.58%) (HR, 1.61, 95% CI, 1.31-1.98).
- There was no significant difference in 1-year rates of hospitalization for heart failure between the lowest hospital volume quartile (9.24%; 95% CI, 7.13%-11.30%) and the highest volume quartile (7.47%; 95% CI, 7.02%-7.92%) (HR, 1.25; 95% CI, 0.96-1.64).
- Among surgeons, adjusted 30-day mortality was increased in the lowest surgical volume quartile (1.53%; 95% CI, 1.24%-1.89%) compared with the highest volume quartile (0.99%; 95% CI, 0.87%-1.13%) (adjusted OR, 2.25; 95% CI, 1.68-3.01).
- Adjusted 30-day composite mortality plus morbidity (defined by bleeding, stroke, prolonged ventilation, renal failure or deep wound infection) was increased in the lowest volume quartile (12.57%; 95% CI, 11.58%-13.65%) compared with the highest volume quartile (9.91%; 95% CI, 9.46%-10.38%) (adjusted OR, 1.72; 95%CI, 1.50-1.98).
The study by Badhwar and colleagues provides guidance on the optimal surgical management of primary mitral regurgitation.
In a perspective article, published in the same issue of JAMA Cardiology, Yogesh Reddy, MBBS, and Rick Nishimura, MD, of the Mayo Clinic, Rochester, Minnesota, weighed in on the identification and treatment of patients with secondary mitral regurgitation, which, until recently, was considered manageable with medical therapy alone.
That changed somewhat with the late 2018 publication of the COAPT trial, “which showed that percutaneous treatment of refractory secondary mitral regurgitation improves symptoms and survival,” they wrote.
“It is clear that severe secondary MR in the setting of new-onset cardiomyopathy frequently resolves with aggressive medical management,” they wrote. “But there remains a subset of patients in whom severe secondary MR persists despite the best existing medical therapy, who may then benefit from correction of the MR.”
Reddy and Nishimura wrote that it is now clear that secondary MR is “pathophysiologically diverse.”
“In patients with ventricular functional MR, aggressive guideline-directed medical therapy (GDMT) should be applied, because many will respond to this therapy alone,” they wrote, adding that other interventions, including catheter-based therapy, may needed in the patients who do not respond.
“It is possible that other forms of secondary MR, such as eccentric ischemic MR or atrial functional MR, in which the anatomical predisposition to MR is somewhat independent of global ventricular remodeling, may be less amenable to GDMT directed toward LV reverse remodeling. These patients require either (1) treatment of a possible reversible causative mechanism (ischemia or atrial fibrillation) or (2) direct intervention or the MR itself,” they wrote.
Reddy and Nishimura concluded that future research should address important unanswered questions regarding secondary MR, including which patients are the best candidates for alternative procedures such as transcatheter mitral valve repair.
-
Greater hospital and surgeon volumes were associated with lower risk-adjusted 30-day mortality, lower 30-day composite mortality and morbidity among patients undergoing surgery for primary degenerative mitral regurgitation.
-
The national study findings could inform quality improvement, patient-physician referral patterns and resource allocation regarding the management of primary mitral regurgitation, the researchers concluded.
Salynn Boyles, Contributing Writer, BreakingMED™
This research was funded by the Society of Thoracic Surgeons.
Lead researcher Vinay Badwar reported receiving nonfinancial support from Abbott Laboratories unrelated to this research. Principal researcher David M. Shahian reported no relevant conflicts of interest. Other researchers reported receiving financial support from pharmaceutical companies unrelated to this research.
Editorial writers’ Yogesh Reddy and Rick Nishimura reported no relevant conflicts of interest.
Cat ID: 308
Topic ID: 74,308,730,308,914,192,925


