Over the last decade, there has been an evolution toward disease-based management approaches for many medical conditions, but some have questioned the appropriateness of this strategy when managing older patients with chronic kidney disease (CKD). It can be challenging for clinicians to manage geriatric individuals with CKD by using disease-oriented models of care because of the prevalence of complex comorbid conditions and syndromes in this patient population. Disease-oriented care models assume a direct causal link between observed signs and symptoms and underlying disease processes. Treatment plans target underlying disease mechanisms and aim to improve disease-related outcomes. In older adults, signs and symptoms often won’t reflect a single underlying pathophysiologic process.
The appropriateness of using disease-oriented models of care has been questioned for elderly patients with CKD because there can be wide variations in life expectancy, functional status, and health priorities in these individuals. Furthermore, the safety and efficacy of recommended interventions are not as well established in older adults with CKD. Disease-oriented approaches may fail to address outcomes that are of greatest concern for patients. They can cause physicians to use treatment strategies that may be inappropriate, which in turn can increase the potential for doing more harm than good.
Benefits of Patient-Centered Care for CKD
More recently, some clinicians have argued that individualized patient-centered models of care may be more appropriate than using traditional approaches in older adults with CKD. By taking an individualized approach, patient preferences are prioritized. Clinicians must also recognize that observed signs and symptoms may not always reflect a single unifying disease process. Signs and symptoms can reflect the complex interplay between pathologic processes, aging, social, psychological, and other factors. Patient-centered care approaches emphasize modifiable outcomes that matter to patients. In many instances, survival may be of less importance to patients than other outcomes, such as quality of life, functional status, pain control, and independence. Under patient-centered approaches, prognostic information relating to these and other outcomes should generally be used to shape treatment decisions rather than dictate them.
26 % of 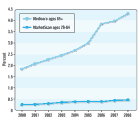 those 60 and older has stage-III CKD
those 60 and older has stage-III CKD
Click here to see the incidence and prevalence of CKD in older adults.
Patient-oriented approaches incorporate information about social support systems and family dynamics, highlighting the role of caregivers. It should be noted that disease-specific diagnoses and management are not abandoned completely. Instead, those principles are incorporated into individualized treatment plans. How they’re incorporated depends on the extent to which disease-based recommendations are aligned with preferences and goals of patients. Individualized treatment plans are intended to be dynamic and bidirectional. They enable clinicians to accommodate changes in health priorities that can occur over time.
Consider the Pros & Cons in Older Adults with CKD
A key advantage to using patient-centered treatment approaches in older adults with CKD is that they embrace the reality that many of these individuals have multiple comorbid conditions in addition to their CKD. Such approaches also recognize the substantial heterogeneity in health status, life expectancy, treatment efficacy, and patient preferences. To support patient-centered approaches in this patient group, clinicians will need to become skilled in the art and science of eliciting patient goals and preferences and then incorporate these into treatment strategies.
Patient-centered approaches to care can result in diverse treatment plans for older adults with similar stages of CKD. Heterogeneity in treatment goals may make it difficult to evaluate the effectiveness of care. In the future, more studies are needed to evaluate the role of patient-centered care in treatment decisions and to determine how these approaches impact outcomes that matter most to patients.



 JonN
JonN