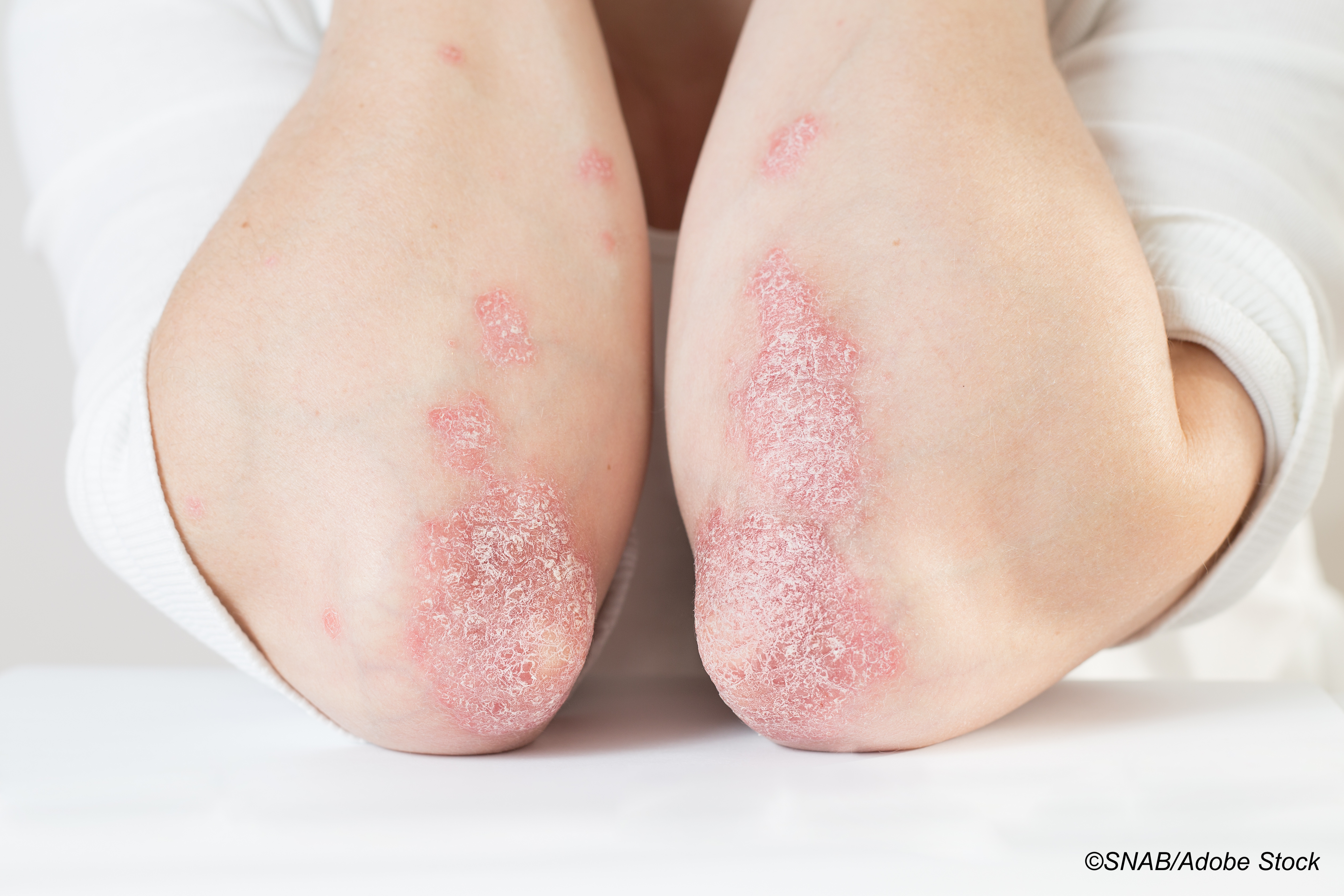
Patients with psoriatic conditions would be willing to engage in—and cooperate with—specialist-led models of care to improve the prevention of cardiovascular disease (CVD), according to a recent double-sided survey of specialists and patients. And on their part, dermatologists who care for these patients reported that they would be willing to engage in risk mitigating strategies such as cholesterol monitoring and statin prescription.
The results are published in JAMA Dermatology.
This willingness and cooperation would go a long way, according to John S. Barbieri, MD, MBA, of Brigham and Women’s Hospital, Boston, and fellow researchers, because patients with psoriatic conditions have a particularly heightened risk of CVD.
“Psoriasis and psoriatic arthritis are chronic inflammatory diseases that are associated with increased risk of cardiovascular disease (CVD) and premature mortality. Patients with psoriasis who require treatment with systemic medications or phototherapy have been reported to have reduced life expectancy by 5 years after adjusting for traditional risk factors. Cardiovascular disease is a leading cause of this excess mortality and guidelines from the American Academy of Dermatology/National Psoriasis Foundation (NPF) and the American Heart Association/American College of Cardiology specifically identify patients with psoriatic disease as a population in need of enhanced CVD prevention efforts,” they wrote.
They noted that while CVD risks are usually managed by primary care physicians (PCPs) and cardiologists, the use of primary care in commercially insured U.S. adults is on the decline, with less than 50% visiting a PCP annually. And, according to a 2020 study from Barbieri and colleagues, almost one-fourth of patients with psoriasis had no encounters with a PCP within a year of their first encounter with a dermatologist.
In the current study, Barbieri and colleagues used electronic surveys to conduct this best-worst scaling study among dermatologists through the National Psoriasis Foundation and the American Academy of Dermatology, who were asked to rank strategies based on their potential to improve the prevention of CVD in patients with psoriatic conditions, as well as about the feasibility of specialist-led screening through an electronically delivered survey from the National Psoriasis Foundation.
In addition, researchers also surveyed patients with psoriasis or psoriatic arthritis about whether they would like specialists to screen for CVD risk factors, and how likely they would be to engage in CVD risk screening and management behaviors in light of recommendations from either their PCP or specialist.
The primary outcomes for both sets of surveys were as follows:
- Clinician surveys: Ratio scaled preference score of strategies that could improve CVD prevention, ranging from 0-100, with higher scores denoting a greater preference; and feasibility of calculating a 10-year CVD risk score and prescribing statins to these patients.
- Patient surveys: Likelihood to check cholesterol levels, incorporate diet and exercise, or use statins as recommended by their PCP or specialists; preference for having specialist(s) educate them about CVD risk; and convenience of having their specialist(s) check cholesterol levels.
For the physician surveys, researchers included 183 dermatologists (55.7% women), more than half of whom (58%) practiced in a single specialty group or solo practice setting. A full 69.3% of them agreed or strongly agreed with the statement “I think checking lipids and calculating a 10-year cardiovascular risk score to determine if a statin is recommended seems doable.” Further, 67.8% of them agreed or strongly agreed that they would change their practice to screen and manage the risks of CVD in these patients if clinical trial data showed better CVD risk prevention with specialist screenings for cholesterol and indications for treatment with statins. However, only 36.1% agreed that prescribing a statin when indicated was feasible.
Among eight different strategies to improve CVD prevention in patients with psoriatic disease, the three that received the highest ranking from dermatologists were as follows:
- Clinical decision support (preference score: 22.3; 95% CI: 20.7-24.0).
- Clinician education outreach (preference score: 15.8; 95% CI: 14.3-17.3).
- Patient educational materials (preference score: 14.1; 95% CI: 12.5-15.7).
Strategies that received the lowest rankings were comparison with peers, pay-for-performance, and mobile app/texting service.
An important caveat is that of the 160 rheumatologists from the NPF and the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis, only 27 completed the survey.
For the patient surveys, Barbieri and fellow researchers included 160 patients with psoriasis and 162 with psoriatic arthritis (mean age: 54 years; 70.2% women), who reported that they were as likely to partake in cardiovascular risk screening and management behaviors whether these were recommended by their PCP or specialist. And 60.0% of patients with psoriasis reported that cholesterol measurement by dermatologists/rheumatologists would be convenient, as did 75.3% of those with psoriatic arthritis.
“In this survey study, dermatologists and patients with psoriatic disease expressed positive perspectives about engaging in a specialist-led model for CVD risk screening and management. More than two-thirds of dermatologists agreed that it was doable to screen for cardiovascular risk factors and nearly half of dermatologists reported that prescribing statins was doable,” concluded Barbieri and colleagues.
In their accompanying editorial, Michael S. Garshick, MD, MS, and Jeffrey S. Berger, MD, MS, both of NYU Langone Health’s Center for the Prevention of Cardiovascular Disease and Leon H. Charney Division of Cardiology, New York, welcomed these results from Barbieri et al, noting that only 35% of patients with psoriasis who are diagnosed with hyperlipidemia receive adequate statin treatment. They added that dermatologists and rheumatologists may be the “only source of contact with the health care system” for these patients.
“[T]he authors propose a clinical care coordinator model whereby data on CVD risk are gathered by the clinician, incorporated into a CVD risk score by a care coordinator, and a protocolized clinician support system helps determine treatment (statin) recommendations,” wrote Garshick and Berger.
“The dermatology and rheumatology communities are at the forefront of treating patients with psoriasis and promoting awareness and research to explain and treat CVD risk in this group who is at risk for early heart disease. The AAD/NPF guidelines were among the first to formally recognize the enhanced CVD risk of patients with psoriasis, with major CV guidelines following shortly thereafter. Moving the needle forward includes refining and developing modifiable CVD risk reduction strategies for patients with psoriasis, and collaboration between the fields of dermatology, rheumatology, and cardiology is key,” they concluded.
Study limitations include the possibility of sampling and response bias, the lack of generalizability to survey nonresponders, a lower incidence of chronic conditions in survey respondents, and the inclusion of only eight potential implementation strategies.
Disclosure:
This study was supported by a grant from the National Psoriasis Foundation Psoriasis Prevention Initiative. The National Psoriasis Foundation participated in the design and distribution of the surveys but had no role in the interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Barbieri is Review and CME Editor for JAMA Dermatology.
Garshick is funded by an American Heart Association Career Development Grant, National Psoriasis Foundation Bridge Grant, and NIH-K23 Career development award.
Berger is funded by grants from the National Institutes of Health.
by
Liz Meszaros, Deputy Managing Editor, BreakingMED™
Kaiser Health News
Kaiser Health News is a nonprofit news service covering health issues. It is an editorially independent program of the Kaiser Family Foundation, which is not affiliated with Kaiser Permanente.

