New research was presented at NLA 2015, the National Lipid Association’s annual scientific sessions, from June 11 to 14 in Chicago. The features below highlight some of the studies that emerged from the conference.
Dyslipidemia in Children With Diabetes
The Particulars: Prior research indicates that dyslipidemia is common in adults with type 2 diabetes. However, few studies have analyzed the type and nature of lipoprotein abnormalities or the determinants of adverse lipoprotein profiles in children with type 2 diabetes.
Data Breakdown: University of Alabama researchers reviewed data on children with type 2 diabetes who underwent standard and/or vertical auto-profile (VAP)-derived lipid profile analyses. Investigators found that BMI was not a determinant of adverse lipid profiles, as most children were in the 95th percentile of weight. However, an A1C higher than 7% was associated with abnormal lipid variables. More than 95% of patients with an LDL higher than 130 mg/dl had an HDL level that was greater than 160 mg/dl.
Take Home Pearls: Weight management and diligent glycemic control appear to be important strategies for mitigating cardiovascular risk in children with type 2 diabetes. An LDL-based treatment cutoff may be sufficient to assess dyslipidemia in this patient population.
Sleep Issues & Coronary Artery Disease
The Particulars: Previous studies have indicated that elevated central apnea index (CAI) scores are common in central sleep apnea that is associated with systolic or diastolic heart failure. However, the relationship between sleep apnea and coronary artery disease (CAD) has not been well established.
Data Breakdown: For a study, researchers analyzed nearly 1,000 patients who were seen at a sleep clinic. The authors found that patients with CAD had more severe obstructive sleep apnea than those without CAD. Patients with CAD slept an average of 287 minutes per night, compared with 315 minutes for those without CAD. Age, dyslipidemia, hypertension, and CAI score were independent predictors of CAD.
Take Home Pearl: Shorter sleep duration and sleep apnea appear to increase the risk of CAD.
Assessing Universal Cholesterol Screening in Youth
The Particulars: Guidelines from the National Heart, Lung, and Blood Institute (NHLBI) recommend universal cholesterol screening for children aged 9 to 11 regardless of their health status or family history. Little is known about how well clinicians adhere to this recommendation.
Data Breakdown: Study investigators conducted a survey of members from the National Lipid Association who were pediatric healthcare providers regarding cholesterol screening and treatment practices. The survey also asked about barriers to university cholesterol screening among children and adolescents. Among respondents, 80% agreed with universal screening, whereas 10% disagreed and 10% were undecided. About two-thirds felt comfortable prescribing a statin to children older than 8 years.
Take Home Pearls: Approximately 20% of pediatric healthcare providers do not appear to follow the NHLBI recommendation of universal cholesterol screening for all children aged 9 to 11. More research is needed to test and develop interventions that are designed to overcome barriers to universal screening in this patient group.
Identifying Familial Hypercholesterolemia Early
The Particulars: Early diagnosis and treatment of familial hypercholesterolemia (FH) has been shown to reduce morbidity and mortality for patients. Studies also show that FH is significantly undertreated in the United States.
Data Breakdown: For a study, researchers implemented an integrated initiative to help identify and treat patients with FH early in the course of the disease. Patients with FH were tagged in electronic health records to increase visibility to all providers. Healthcare providers received communications regarding the initiative, and patients were sent letters notifying them of their condition. The rate of FH identification in patient charts increased from 13.0% prior to the initiative to 95.4% after letters were received and provider encounters occurred. In addition, treatment for FH increased from 90.3% to 98.5% over the study period.
Take Home Pearl: A novel outreach method using electronic health records and enhanced communication strategies appears to successfully increase the identification of FH and treatment for the disease.
Assessing ASCVD Risk by Race
The Particulars: The incidence and prevalence or atherosclerotic cardiovascular disease (ASCVD) in the United States varies by race, according to previous research. However, the predominance of ASCVD-related risk factors by race have not been well described.
Data Breakdown: Study investigators compared cardiometabolic risk factors among African-American, Latino-Hispanic, and Caucasian patients who underwent a fasting lipid panel followed by therapy initiation and repeat testing between 3 and 12 months after their initial visit. The following distribution of risk factors by race was observed: 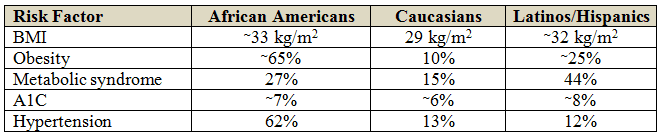
Take Home Pearls: The distribution of risk factors known to cause ASCVD appears to vary according to race. Race appears to be an important variable to take into consideration when developing strategies to optimize risk in patients with ASCVD.


