Older adults who show patterns of chronically high and increasing depressive symptoms over time may be at higher risk of subsequently developing dementia.
Previous studies have suggested that there appears to be a link between depressive symptoms and the onset of cognitive decline and dementia. “Some research suggests older adults may develop depressive symptoms as a reaction to experiencing cognitive decline, but other investigations have identified depression as a risk factor for dementia,” explains Allison R. Kaup, PhD. Further complicating the understanding of these associations is that experts have theorized that depressive symptoms and cognitive decline may both be symptoms of an underlying neurodegenerative process.
According to Dr. Kaup, most of the studies looking at the link between depressive symptoms and the development of dementia have been limited because they only measure depressive symptoms at one time point. “This fails to capture some of the variability in symptoms and the long-term course of depression,” she says. “This information may be important because older people appear to experience different patterns of depressive symptoms over time.” Currently, it is unclear if different trajectories of depressive symptoms confer differential risk for dementia.
Examining Trajectories
For a study published in JAMA Psychiatry, Dr. Kaup, Kristine Yaffe, MD, and colleagues looked at the association between trajectories of depressive symptoms and the risk of dementia among older adults who were followed prospectively as part of the Health, Aging, and Body Composition study. The settings included community research centers located in Memphis, Tennessee, and Pittsburgh, Pennsylvania. The trajectory of depressive symptoms was assessed from baseline to 5 years out among 2,488 black and white older adults with repeated depressive symptom assessments who were free of dementia throughout that period.
Related Articles
- Hypertension Onset After Age 80 May Protect Against Dementia
- Dementia May Be Exacerbated by Hospital-Related Delirium
- Continuing Warfarin Protective After Diagnosis of Dementia
- Acupuncture Boosts Effectiveness of Standard Medical Care for Chronic Pain, Depression
The researchers also investigated whether the effect of depressive symptom trajectories on dementia risk differed by sex, race, and if patients carried the APOE. Some evidence suggests that depression and its association with dementia may differ by these factors. In addition, the authors looked at whether depressive symptom trajectories provide information about the risk of dementia beyond what was captured by one-time assessments of depressive symptoms.
Assessing Results
Overall, the study found that 14.2% of participants developed dementia at an average of 3.9 years after the depressive symptom assessment period. “Older adults with patterns of moderate and increasing depressive symptoms and those with high and increasing symptoms were more likely to develop dementia than those with consistently minimal symptoms,” Dr. Kaup says. However, only patients with a trajectory of high and increasing depressive symptoms remained at statistically greater risk of developing dementia after accounting for other factors. These patients were almost twice as likely to develop dementia even after adjusting for cognitive functioning at the time of their depressive trajectories (Figure below).
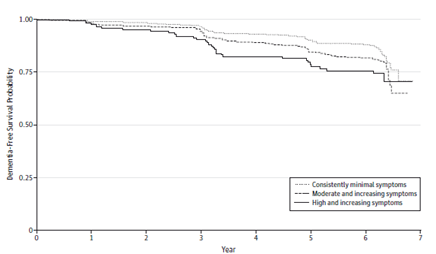
The figure below depicts the association between depressive symptom trajectory and dementia-free survival among 2,488 older adults.
It is difficult to determine if depression is a risk factor for dementia, a symptom of an underlying neurodegenerative processes, or some combination of the two, according to the study. “Our results suggest that the nature of the depression-dementia relationship may be different depending on the pattern of depressive symptoms,” says Dr. Kaup. It is possible that some older adults with depressive symptoms were experiencing those symptoms as an emotional response to already being in the early stages of cognitive decline. On the other hand, a pattern of chronically high and increasing depressive symptoms appears to increase risk for subsequent cognitive decline.
In addition, the analysis revealed that dementia risk did not appear to be strongly related to simply having high baseline depressive symptoms or high symptoms at the most recent time point. Instead, the researchers observed a pattern of depressive symptoms that were both chronically high and increasing over time, a finding that appeared to be particularly impactful with regard to increasing dementia risk.
Important Implications
More research is needed to clarify whether the mechanisms driving the associations between depressive symptoms and dementia may differ depending on the pattern of depressive symptoms that individuals experience over time. The study group noted that few participants in the study were taking antidepressants and that they did not have information about whether or not patients were receiving non-pharmacologic interventions for depression. As a result, they were unable to thoroughly investigate the potential effect of treatment for depression.
“We hope that future research will be conducted to determine if effective depression interventions can also reduce risks for dementia,” says Dr. Kaup. “In the meantime, our findings emphasize the importance of screening for and tracking depressive symptoms among older adults over time. Our findings may also provide extra motivation for physicians to encourage older patients to take up healthy lifestyles as a way to protect brain health as much as possible.”



 PhysWeekly
PhysWeekly