An article in last week’s Newsweek magazine says it is. “Artificial intelligence will cure America’s sick health care system” using data and automation to “drive down the costs of health care while increasing effectiveness.”
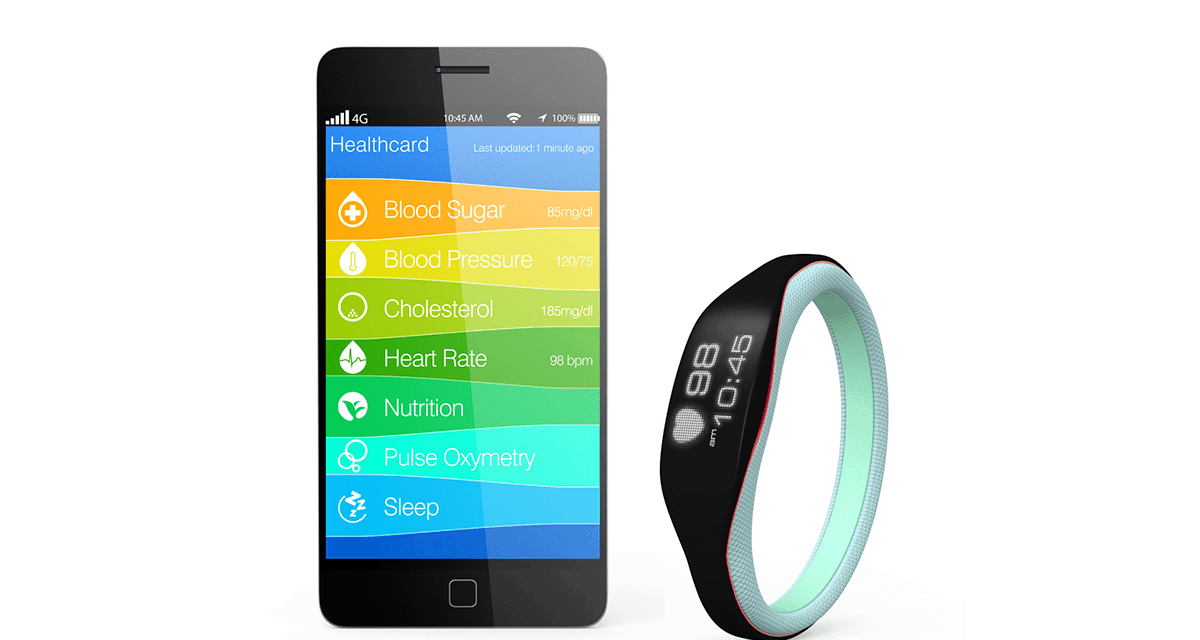
According to Newsweek, it will work like this for diabetes. A company called Virta Health has come up with a smartphone app that is like “a live-in doctor and diabetes coach.” Type 2 diabetics who enroll will enter data such as blood sugar levels, weight, blood pressure, and activity manually or using automated devices like Fitbit. The app will also ask patients about their moods, energy levels, and hunger.
Artificial intelligence at Virta will analyze the data and suggest changes in diet, drugs, or behavioral counseling, which will be vetted by a doctor and given to the patient.
Proof that the product works was demonstrated in a recently published study from Virta and Indiana University.
The patient population consisted of 238 morbidly obese patients with type 2 diabetes; 90% were taking one or more diabetes medications, and 80% had hemoglobin A1c levels > 6.5%. Values < 6.5% indicate tight glucose control.
The major intervention was a low carbohydrate [< 30 g per day] diet to induce “nutritional ketosis.” Serum levels of the ketone beta-hydroxybutyrate were monitored frequently.
Patients were followed for 10 weeks after enrolling, and the following statistically significant results were noted:
– Mean hemoglobin A1c fell by 1%.
– Patients with hemoglobin A1c levels > 6.5% fell to 44%.
– At least one diabetes medication dose was lowered or eliminated in 57% of patients.
– Body mass index decreased by 7% from a baseline of 40.7 kg/m2 to 37.7 kg/m2.
No patient suffered diabetic ketoacidosis.
Looks pretty good, doesn’t it? But they don’t call me “skeptical” for nothing. Here are some problems with this study.
It was funded by Virta and described by the authors as “a nonrandomized demonstration study.”
The paper was published in JMIR (Journal of Medical Internet Research) Diabetes, an open access journal not listed in PubMed.
Subjects “were recruited via clinical referrals, media advertising, and word-of-mouth.” Therefore they were more likely to have been motivated to participate.
Caloric intake was individualized for each patient and was not reported in the study’s results.
The length of patient follow-up was only 10 weeks. Other low carbohydrate ketogenic diets such as the Atkins diet are known to have poor adherence. A small randomized trial of the Atkins vs. a conventional diet in the New England Journal of Medicine found 41% of patients had dropped out of the study after 12 months. The authors concluded, “Adherence was poor and attrition was high in both groups.”
We are going to need a better study with randomized patients and a much longer follow-up period before we can say artificial intelligence is going to “cure America”s sick healthcare system.”
Skeptical Scalpel is a retired surgeon and was a surgical department chairman and residency program director for many years. He is board-certified in general surgery and a surgical sub-specialty and has re-certified in both several times. For the last six years, he has been blogging at SkepticalScalpel.blogspot.com and tweeting as @SkepticScalpel. His blog has had more than 2,500,000 page views, and he has over 15,500 followers on Twitter.


 Janine Anthes
Janine Anthes