Many clinicians are taking to social media to debunk false information and mistaken opinions regarding vaccines, and our analysis of activity on Twitter shows that there is benefit to this, but that to shift public opinion and improve vaccine adoption to herd-immunity levels may take one-on-one in-person discussion.
A US Senator compared vaccines to sorcery.
You can be forgiven if you had thought we were talking about some of the vocal members of the “Anti Vaccination Society of America” circa 1879, but actually, we are referring to Rep. Jonathan Stickland of Texas in 2019.
This blog draws from analysis of nearly 5,000 tweets taken from discussion threads over a period in March and April 2019. Using the participant-observer research approach, we engaged in discussions of vaccines on Twitter for several weeks, and what we observed falls into three basic causative dynamics: Affiliation, Simplification, and Trust. The bottom line as far as treatments for antivax belief goes, is that some people can indeed be brought back to the light, but it cannot be done by force of argument and logic alone.
We monitored several hashtags (Figure 1), as well as a few highly popular Tweet threads.
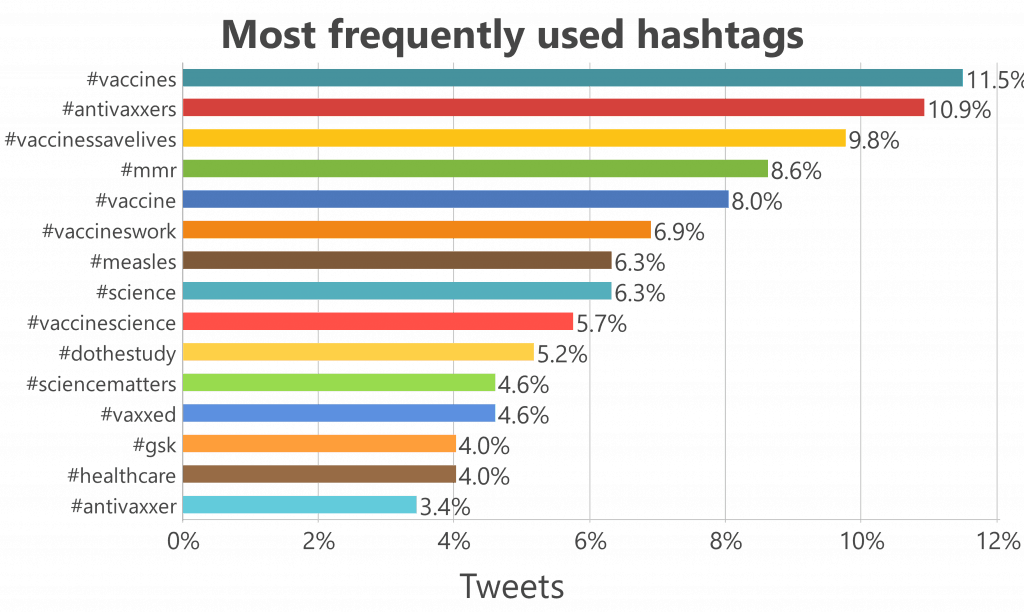
Figure 1: Hashtag Scope
Affiliation
What became clear from the analysis was that people were forming an attitude toward vaccines through the lens of affiliation—that is, “how do people like me feel about vaccines” rather than the strictly factual and medical position of the leading science bodies, or their physician. This “people like me” dynamic reflects on research of ingroup vs outgroup behavior. One particularly relevant body of research into this is the work done by Muzafer Sherif (eg, the “Robber’s Cave” experiment on conflict and group behavior).
Simplification
Infectious diseases, immune response, and epidemiology are complex subjects, and how exactly a vaccine gives rise to variable and imperfect herd immunity is not something in which the typical layman has deep insight. Further, the cognitive dissonance of experts saying one (complex) thing while celebrities and friends say another (simple) thing easily leads to a desire to simplify the arguments down to easily digestible chunks. One such chunk, mediated by group affiliation, is that vaccines are complicated and artificial, while measles parties are simple and natural.
Which brings us to trust.
Trust
We observed that people were basing the degree and specifics of what messages they accepted on a matter of whether they trusted the source. Trust of the bearer of a message seems to be more indicative of acceptance than the content of the message itself. Antivaxxers distrusted pharmaceutical companies and trusted personal accounts of harm. Those who were pro-vaccine, in turn, trusted scientific sources such as the CDC, experts in the field of infectious diseases, and people who had science backgrounds who were positive toward vaccines. Trust was observably sticky and communicable—if a trusted source cited another source, that source inherited trust on the whole, and once trusted, they were regarded as in-group. This mechanism powerfully channeled acceptance down a path in a social network.
The Mechanism
Overall, group affiliation mediates who we trust, and simplification what exactly we trust, but there is a recursive mechanism at play here. The recursion may start with “who is in my group” shift to simplification of a message, then to a review of whether the person or group behind the message is trusted, and back to a resorting and reclassification of “who is in my group.” Some people described initial distrust due to a negative experience, such as an adverse drug event. This event may have happened to themselves, to family or friends, but might also be vicariously inferred through anecdotes about more distant connections or sources reported by family or friends.
A second source of distrust was unrelated to vaccines but rather to general social presentation. For example, the scandals of price-fixing and price-hiking of drugs like insulin result in highly negative social presentation of drug companies. Every news article about Martin Shkreli may have corroded public trust in pharma companies across the board.
Likewise, news regarding adverse outcomes of drugs also chipped away at trust in pharma as an entire industry—the role of Purdue in the opioid crisis, the public impression of heart risks due to Rofecoxib (Vioxx), and the legendary case of Thalidomide.
This mounting distrust in an entire industry, via simplification and affiliation, feeds a process of incremental assignment and dis-assignment of trust and affiliation in a way that logically leads to an outcome in which Andrew Wakefield may be highly trusted and regarded as in-group, while a primary care physician may become out-group and distrusted.
Engagement in Social Media
The degree to which clinicians were active in the Twitter discussions was remarkable. Participant “A” in Figure 2, for example, was a physician, and several physicians were actively engaged in debunking false claims, routing people to reputable sources, and providing support to other clinicians in the discussions. The clinicians were professional, and almost always courteous, but faced responses by antivaxxers that ranged from questioning their integrity to outright insults and threats.
From the evidence of the Twitter data, it does not seem that anyone changed their position, although it was clear that some of the antivaccine group shifted somewhat, and that pro-vaccine people refined their understanding of the facts and issues, and gained far greater vocabulary of the issues and much better arguments.
The benefits may thus include developing a larger number of pro-vaccine laypeople armed with greater understanding of the issues, a repertoire of evidence-based arguments, and a library of trustworthy sources for further information. This may help to sway fence-sitters in the public, moderate antivaxxers’ opinions, and inoculate (sic) others in their social network against infection by antivaxx memes.
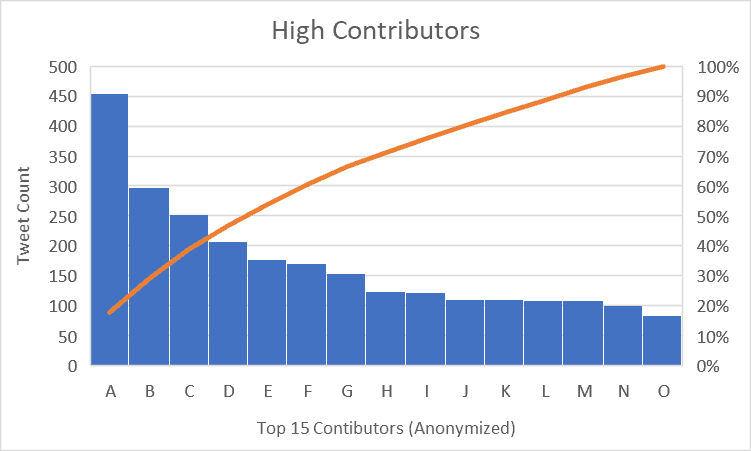
Figure 2: Sample of Participation (One Week)
Next Steps
Given that we saw very little shift in opinions in the Twitter data, it may be best to regard social media as a beneficial way to help the army of pro-science laypeople, but that shifting the needle on vaccine acceptance may require in-person contact. This may mean un-simplifying the facts, and being specific about a vaccine in order to combat the overall low opinion many people have of pharma as an industry. For example, in direct discussion with patients, it may help to uncouple a specific MMR vaccine from the general buzz against pharma. Perhaps specific clinician feedback to a patient that THIS vaccine is effective, trustworthy, and cost/effective in terms of risk, would be more effective in shifting opinion and adoption.
Our advice is that if you have the energy and don’t mind being sworn at occasionally, being actively pro-vaccine on social media is a socially worthwhile activity, and does help, but that if you would rather work at the individual patient level, or feel up to holding a small patient-education sessions at your practice, this may be more effective in shifting the needle on those people’s opinions and acceptance of vaccines.


 PWeekly
PWeekly

