Avacopan — a small-molecule C5a receptor antagonist — works to block not only C5a via the C5a receptor, but neutrophil chemoattraction and activation as well. In a previous phase II trial, avacopan was shown to have efficacy against vasculitis, and, in a previous animal modelling study of ANCA-associated vasculitis, it was effective in preventing glomerulonephritis.
“Activation of the alternative complement pathway, which results in terminal C5a production, is a component of the pathogenesis of ANCA-associated vasculitis,” wrote lead author David R.W. Jayne, MD, of Addenbrooke’s Hospital, Cambridge, U.K., and colleagues.
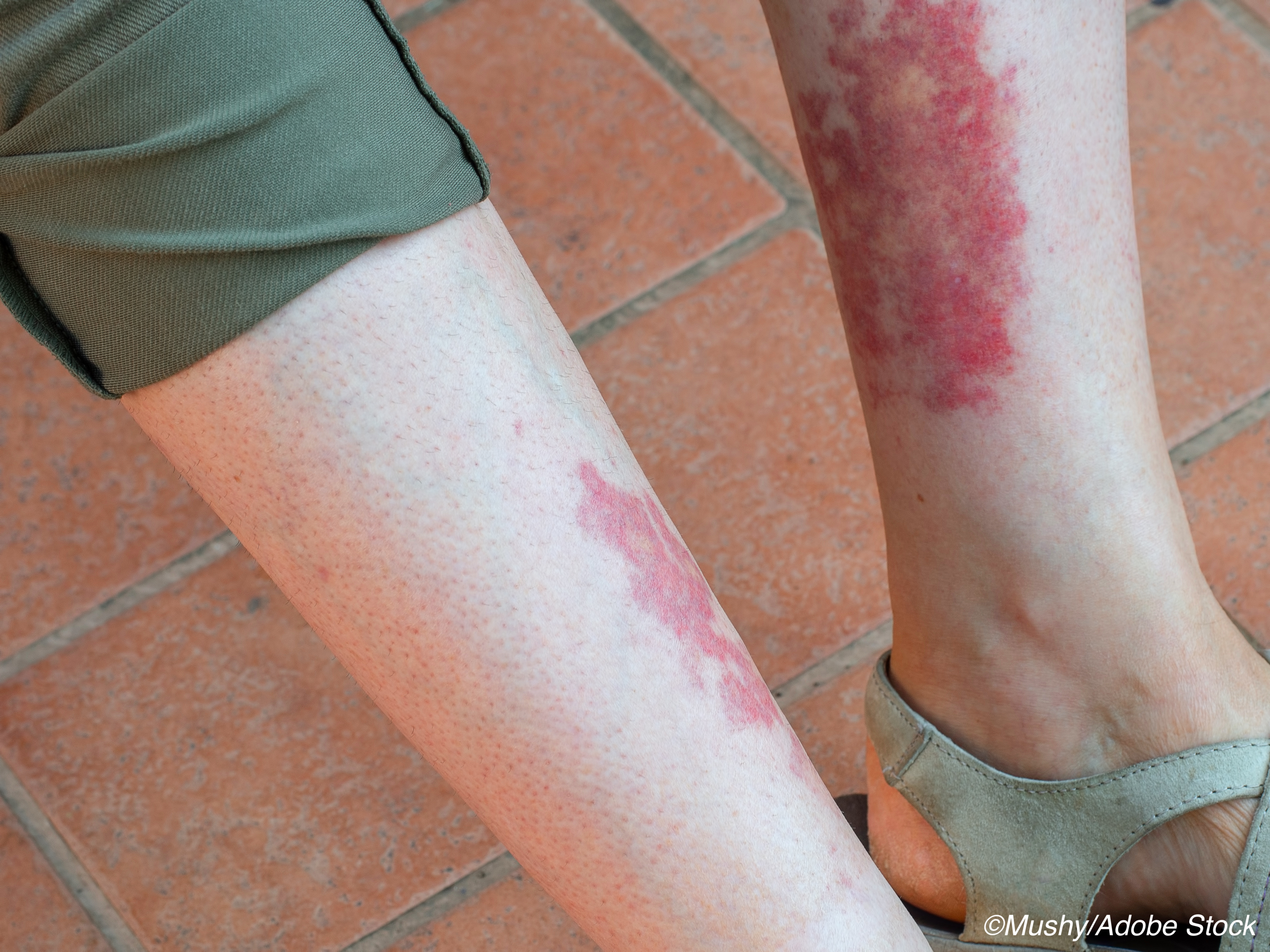
“Patients with ANCA-associated vasculitis may have life-threatening complications, including impairment in kidney function caused by progressive focal necrotizing glomerulonephritis. ANCA-associated vasculitis can also result in deterioration of health-related quality of life because of organ damage, as well as toxic effects from medications used to treat the disorder, including from long-term use of glucocorticoids,” they noted.
In the international, double-blind, double-dummy, randomized, controlled ADVOCATE study, Jayne and fellow researchers randomized 331 patients (mean age: 61 years; 53.7% to 59.0% male) with ANCA-associated vasculitis to treatment with oral avacopan (30 mg bid) plus prednisone-matching placebo or a tapered oral prednisone plus an avacopan-matching placebo. All patients were also treated with either cyclophosphamide followed by azathioprine or rituximab.
At week 26, remission occurred in 72.3% of patients treated with avacopan, compared with 70.1% of those treated with prednisone (estimated common difference: 3.4 percentage points; 95% CI −6.0 to 12.8; P<0.001 for noninferiority; P=0.24 for superiority). At week 52, sustained remission occurred in 65.7% versus 54.9%, respectively (estimated common difference: 12.5 percentage points; 95% CI 2.6-22.3; P less than 0.001 for noninferiority; P=0.007 for superiority).
Treatment with avacopan led to significant reductions in the severity of glucocorticoid-induced toxic effects at week 26 — a secondary endpoint of the study. The least-squares mean in the Glucocorticoid Toxicity Index Cumulative Worsening Score (GTI-CWS) — in which higher scores indicate greater severity of toxic effects — was 39.7 in the avacopan group, compared with 56.6 in the prednisone group (difference: −16.8 points; 95% CI −25.6 to −8.0). Similarly, the least-squares mean for the GTI-Aggregate Improvement Score (AIS; again, higher scores indicate greater severity of toxic effects) at the same timepoint showed significantly greater improvement in patients treated with avacopan versus those treated with prednisone (11.2 versus 23.4, respectively; difference: −12.1; 95% CI −21.1 to −3.2).
Serious adverse events were seen in 37.3% of patients in the avacopan group compared with 39.0% of the prednisone group. The most common of these was vasculitis worsening, which occurred in 10.2% versus 14.0%, respectively. Serious infections occurred in 13.3% versus 15.2%, and liver-function abnormalities in 9 versus 6 patients, but all were resolved upon discontinuation of the trial medication.
“The number of serious adverse events (excluding events of worsening vasculitis) was 33% higher in the prednisone group than in the avacopan group, a finding consistent with a higher exposure to glucocorticoids in that group, and there were more deaths, life-threatening or serious adverse events, and infections in the prednisone group than in the avacopan group,” noted these researchers.
In an accompanying editorial, Kenneth J. Warrington, MD, of the Mayo Clinic College of Medicine and Science, Rochester, Minnesota, praised the researchers’ use of glucocorticoid toxicity as an end-point, albeit it secondary.
“An innovative aspect of the ADVOCATE trial was the use of a Glucocorticoid Toxicity Index that captures common glucocorticoid-related toxic effects, including change in body weight, glucose tolerance, blood pressure, lipids, myopathy, neuropsychiatric features, and infection. Using this tool, the investigators found that patients in the avacopan group had fewer glucocorticoid-related adverse events. Given concern about the potential risk of infections related to complement inhibition by avacopan, it is noteworthy that 13% of the patients in the avacopan group and 15% of those in the prednisone group had serious infections, but no Neisseria meningitidis infections occurred,” Warrington wrote.
“The ADVOCATE trial heralds a change in the treatment of ANCA-associated vasculitis that was previously unthinkable — the possibility of inducing disease remission without glucocorticoids. However, patients in this trial did receive a brief course of glucocorticoids during the screening phase or early in the trial as prednisone was being tapered off and could receive glucocorticoids as rescue medication. The average total prednisone-equivalent glucocorticoid dose was approximately 1.3 g (equating to 4 mg per patient per day) in the avacopan group and approximately 3.7 g (12 mg per patient per day) in the prednisone group,” he added.
These results will — hopefully — pave the way to the study of other complement-directed treatments for ANCA-associated vasculitis, continued Warrington, adding that a phase II trial is currently underway to assess the efficacy of IFX-1, a monoclonal antibody against the C5a molecule. Also noteworthy, he wrote, are recent case reports that suggest that eculizumab may be effective for refractory ANCA-associated vasculitis.
“The ADVOCATE trial is a milestone in the treatment of ANCA-associated vasculitis; complement inhibition with avacopan has glucocorticoid-sparing effects and results in superior disease control,” Warrington concluded.
-
Orally administered avacopan is effective in patients with ANCA-associated vasculitis without daily oral prednisone treatment.
-
Avacopan was noninferior but not superior to tapered prednisone at inducing remission at week 26 and superior to prednisone with maintaining sustained remission at week 52.
Liz Meszaros, Contributing Writer, BreakingMED™
This study was supported by ChemoCentryx.
Jayne reported receiving consulting fees from AstraZeneca, ChemoCentryx, and Genentech and grant support, paid to the University of Cambridge, and consulting fees from GlaxoSmithKline.
Warrington reported grants from Eli Lilly, grants from Kiniksa, grants and personal fees from Roche/Genentech, personal fees and non-financial support from Sanofi, grants from GlaxoSmithKline, outside the submitted work;
Cat ID: 190
Topic ID: 79,190,730,190,192,925


