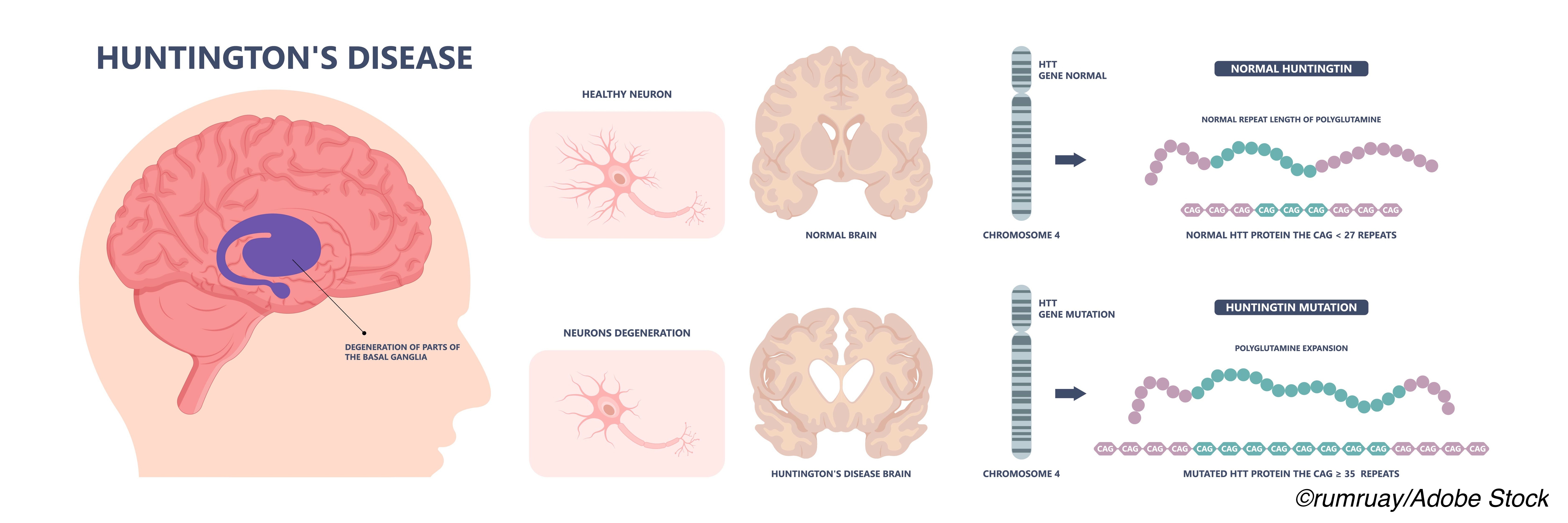
Patients presenting with Huntington’s disease (HD) at older ages were more likely to have motor difficulties as their initial symptom and less likely to have initial psychiatric symptoms, a retrospective registry study found.
Huntington’s disease is a central neurodegenerative disorder caused by an expanded CAG repeat (>35 CAGs) in the huntington gene. Longer repeats have been associated with earlier disease onset. The movement disorder usually includes chorea. In this analysis, although age of onset of any HD symptom correlated with pathologic CAG repeat length, the identity of the first symptom was independent of CAG repeat length, reported Thomas Massey, MA, BM BCh, DPhil, of Cardiff University in the United Kingdom, and co-authors, in Neurology.
“In this large study of over 6,000 patients, we have shown that the initial manifestation of HD, as determined retrospectively by an expert rater, varies significantly with age,” the researchers wrote.
“Depression usually had the youngest mean age at onset, followed by motor impairment and then apathy and cognitive impairment as the latest symptoms,” they added. “Late presentations (>60 years) are usually associated with motor abnormalities, whereas early presentations (<20 years; juvenile HD) are associated with a wider range of motor, cognitive and psychiatric abnormalities.”
The researchers analyzed data from 6,316 patients with genetically verified HD with CAG lengths of 36-93 repeats from the European REGISTRY study. Age at symptom onset was determined with the HD Clinical Characteristics Questionnaire (HD-CCQ), which was completed by a healthcare professional. Patients reported age of onset for eight common symptom categories, if applicable: motor (chorea or other), cognitive impairment that affected work or daily life, apathy, depression, perseverative/obsessive behavior, irritability, violent or aggressive behavior, and psychosis. Symptoms were grouped as motor, psychiatric, and cognitive.
Patients with onset before age 20 (juvenile HD) presented with varied features, including motor (24.5%), cognitive (21.8%), and psychiatric (28.2%).
In adult-onset HD, the initial manifestation was more likely to be motor than psychiatric, and likelihood increased with age. Per 10-year increase in onset age, OR for motor onset was 1.06 (95% CI 1.04-1.07, P=7.4 x 10-22) while psychiatric presentations became less likely (OR 0.96, 95% CI 0.95-0.97, P=9.4 x 10-16).
In patients with onset over age 60, 68.6% had initial motor abnormalities; psychiatric (11.5%) or cognitive (6.7%) presentations were fewer.
No significant relationship was seen between CAG length (36-59 inclusive) and proportions of motor, cognitive and psychiatric onset, but a strong inverse correlation between CAG repeat length (40-55 inclusive) and mean age at symptom onset was seen for all symptoms analyzed in the study.
“Importantly, our results show there is little relationship between pathogenic CAG repeat length and onset type in adult-onset HD, despite both being associated with age at clinical onset,” Massey and colleagues wrote. “These data fit a model in which age at clinical onset is driven primarily by CAG repeat length, but modified by environmental factors and variants at other genomic loci.”
In an accompanying editorial, Elizabeth Anne McCusker, MBBS, and Clement Loy, MBBS, PhD, both of the University of Sydney in Australia, wrote, “This study confirms findings from other studies, including the valuable longitudinal premanifest studies, Predict HD, PHAROS, and Track HD.”
“Changes were identified more than 10 years ahead of clinical motor diagnosis, including changes in cognition and MRI volumetric imaging,” McCusker and Loy continued. “In general, the conclusions would be that HD is rarely unimodal, even at first diagnosis.”
Earlier research comparing late versus early onset Huntington’s disease suggested that motor deficits were worse for late-onset patients during an early stage of manifest disease, but worse for young onset patients at later stages. A 2019 analysis of REGISTRY data comparing late (>59) and earlier-onset HD found late-onset patients more frequently presented with gait and balance problems.
Data for the present study were collected from June 2004 to February 2016. The cohort was 48.8% male, and mean age at the most recent clinic visit was about 53.
Lifetime prevalence was high for motor symptoms, which were present in >99% of participants; 96.8% had chorea. Depression was the second most common symptom, occurring in 64.5% overall and more likely in females than males (70.4% vs 58.2%, respectively; OR 1.70, 95% CI 1.52-1.90, P=2.6 x 10-21). Cognitive impairment and apathy were equally likely in males and females (about 58%), but there was significantly more irritability observed in males (62.9% vs 56.9%, OR 0.78, 95% CI 0.70-0.87; P=4.0 x 10-6). Violent or aggressive behavior was also more likely in males (34.9% males vs 27.0% females, OR 0.69, 95% CI 0.62-0.77; P=2.0 x 10-10). Psychosis was the least prevalent (about 11%) in both males and females.
The presence of any psychiatric or cognitive symptom was significantly associated with lower total functional capacity with work and independent functioning, most significantly for cognitive impairment.
“Psychiatric symptoms are common in HD gene carriers and are associated with CAG repeat length,” Massey and colleagues wrote. “As it is impossible to distinguish confidently between non-motor symptoms arising from HD and primary psychiatric disorders, particularly in younger pre-manifest patients, non-motor symptoms should not be used to make a clinical diagnosis of HD.”
Limitations include retrospective data recorded from the most recent clinic visit, which is at different points in the disease course for different patients. Data also are subject to recall bias.
-
Patients presenting with Huntington’s disease at older ages were more likely to have motor difficulties as their initial symptom and less likely to have initial psychiatric symptoms, a retrospective registry study found.
-
Patients with Huntington’s onset before age 20 presented with a variety of motor, cognitive, and psychiatric features.
Paul Smyth, MD, Contributing Writer, BreakingMED™
The REGISTRY is supported by the European Huntington’s Disease Network.
Massey was supported by the Welsh Clinical Academic Track Fellowship, MRC Clinical Training Fellowship, and Patrick Berthoud Charitable Trust Fellowship through the Association of British Neurologists.
The editorialists reported no relevant disclosures.
Cat ID: 130
Topic ID: 82,130,730,130,192,925


