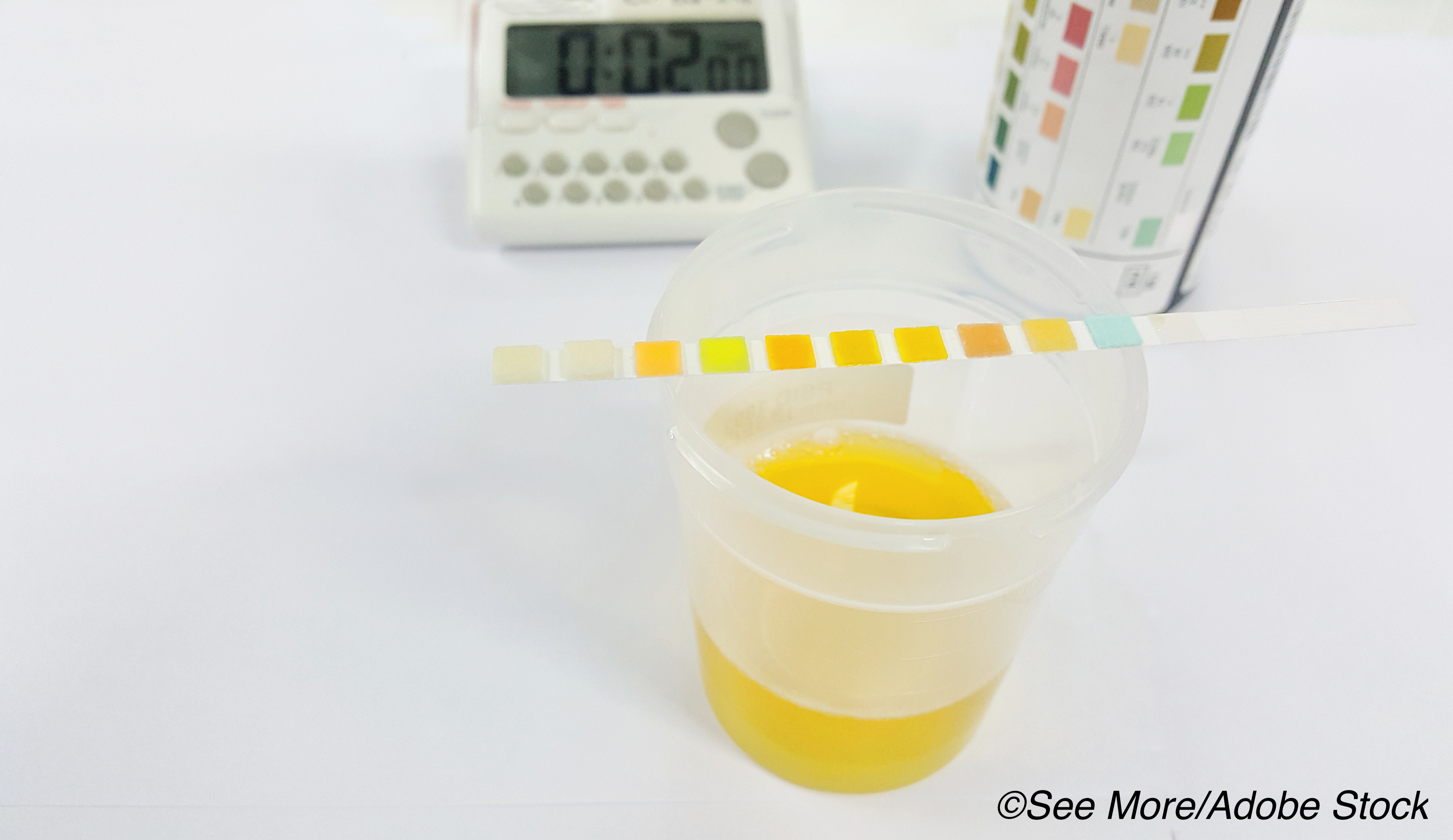
An alternative method for screening and staging chronic kidney disease, which utilizes protein-creatinine ratio (PCR) or urine dipstick protein, may prove to be a clinically useful and cheaper alternative to measuring albuminuria in the urine, researchers report.
The researchers developed equations designed to convert urine PCR and urine dipstick protein to albumin-creatinine ratio (ACR) values, based on data from their participant-based meta-analysis involving more than 900,000 adults.
The empirically developed equation for converting PCR to ACR corresponded well with threshold estimates in current guidelines for the staging of chronic kidney disease (CKD), wrote researcher Keiichi Sumida, MD, PhD, and colleagues with the Chronic Kidney Disease Prognosis Consortium.
“Our PCR conversion equations demonstrated relatively high specificity and sensitivity for detecting CKD stage A2 and higher, and the 2-year kidney failure risk equation (KFRE) using predicted ACR performed similarly to that using observed ACR,” they wrote in Annals of Internal Medicine, published online July 13.
“Although further testing is required to establish the robustness and utility of these equations, our results suggest that if ACR is not available, predicted ACR may be useful and informative for harmonization across research studies, CKD screening and classification efforts, and use in risk prediction equations.”
While urine albuminuria measurement is considered the gold standard for quantifying urinary protein to diagnose and stage kidney disease and predict kidney failure, total urine PCR or dipstick protein is often substituted due to lower cost and wider availability.
Single studies have examined the relationship between PCR or urine dipstick protein categories and urine ACR, but “the diagnostic performance of these thresholds and the consistency of relationships across several cohorts and health systems have not been established,” Sumida and colleagues wrote.
Their individual participant-based meta-analysis of 33 clinical and research cohorts from the international Chronic Kidney Disease Prognosis Consortium (CKD-PC) included 919, 383 participants who had both ACR and either PCR or urine dipstick measured on the same day. More than half the patients had diabetes, and nearly three-quarters had hypertension.
The equations developed by the researchers were tested for purposes of CKD screening (ACR ≥30 mg/g) and staging (stage A2: ACR of 30 to 299 mg/g; stage A3: ACR ≥300 mg/g).
Median ACR was 14 mg/g (25th to 75th percentile of cohorts, 5 to 25 mg/g), and the investigation found the association between PCR and ACR to be inconsistent for PCR values less than 50 mg/g.
For screening (ACR>30 mg/g), the PCR conversion equations demonstrated moderate sensitivity (91%) and specificity (87%). For classification into stages A2 and A3, the PCR conversion equations also demonstrated moderate sensitivity (75% and 87%, respectively) and specificity (89% and 98%, respectively).
Urine dipstick categories of trace or greater, trace to +, and ++ for screening for ACR values greater than 30 mg/g and classification into stages A2 and A3, respectively, had moderate sensitivity (62%, 36%, and 78%) and high specificity (88%, 88%, and 98%).
“For individual risk prediction, the estimated 2-year 4-variable kidney failure risk equation using predicted ACR from PCR had discrimination similar to that of using observed ACR,” the researchers wrote.
For PCR measures greater than 50 mg/g, adjusted modeling showed a 2.99-fold increase in predicted ACR for each doubling of PCR in the range of 50 to 500 mg/g. No consistent relationship was observed at values below 50 mg/g.
In an editorial published with the study, Tyrone Harrison, MD, and Brenda Hemmelgarn, MD, PhD, of the University of Calgary, Alberta, Canada wrote that a major strength of the research is the generalizability to many clinical settings.
A study limitation was the difference in laboratory assays used, which may have contributed to variation among cohorts.
“This limitation was identified as an important modifying variable in previous studies,” they wrote. “These equations should not be used in the evaluation of patients with diseases expected to have less prominent albumin proportions (such as low-molecular weight proteinuria in the setting of myeloma).
The editorial writers concluded that “the implications of accurate and high-performing equations to estimate ACR from urine protein measures are immense.”
“As suggested by Sumida and colleagues, as well as the KDIGO guidelines, the reagent costs to measure protein are considerably less than those for measuring albumin; therefore, it is highly likely that in some health care systems, only PCR or urine dipstick measures are available. In this setting, use of conversion equations from the inexpensive and widely available PCR or dipstick gives patients and clinicians in economically disparate locations access to such tools as the KFRE.
“Use of these equations in research is another important application. For example, retrospective cohort studies that use large administrative health databases may use these conversion equations to account for and estimate missing ACR data.”
-
An alternative method for screening and staging chronic kidney disease, which utilizes protein-creatinine ratio (PCR) or urine dipstick protein, proved effective in estimating albumin-creatinine ratio.
-
The empirically developed equation for converting PCR to ACR corresponded well with threshold estimates in current guidelines for the staging of chronic kidney disease.
Salynn Boyles, Contributing Writer, BreakingMED™
This research was funded by the National Institute of Diabetes and Digestive and Kidney Diseases and the National Kidney Foundation.
Sumida disclosed no relevant relationships.
Harrison and Hemmelgarn disclosed no relevant relationships.
Cat ID: 127
Topic ID: 81,127,254,570,730,127,192,925