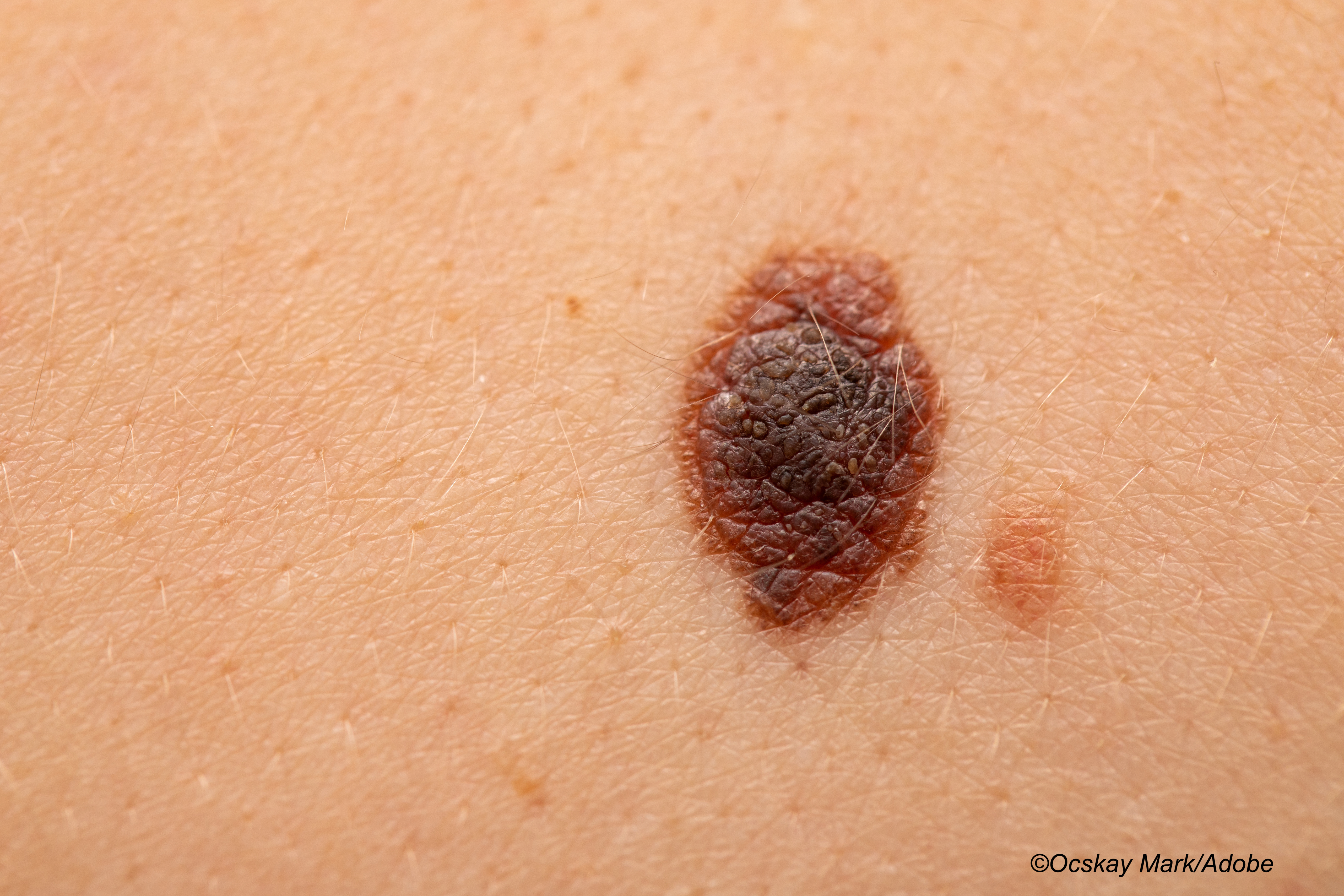
A modified prognostic nodal classification system based on comprehensive nodal burden seemed capable of accurately stratifying mortality risk in patients with cutaneous melanoma, according to results from a retrospective analysis of two independent databases.
In a cohort of 105,785 patients with cutaneous melanoma undergoing surgery and nodal evaluation, the proposed nodal schema showed progressively increasing mortality, with 3-year overall survival (OS) rates as follows:
- NO (0 positive lymph nodes): OS rate 89.9% (95% CI. 89.6-90.1%).
- N1a (1 clinically occult positive lymph node): OS 79.2% (95% CI, 78.3-80.1%).
- N1b (2-3 clinically occult positive lymph nodes or 0 positive lymph nodes with in-transit metastasis): OS rate 69.7% (95% CI, 68.2-71.3%).
- N2a (1 clinically detected positive lymph node or 1 clinically occult positive lymph node with in-transit metastasis): OS rate 58.9% (95% CI, 56.4-61.6%).
- N2b (2-3 clinically detected positive lymph nodes with or without in-transit metastases): OS rate 52.4% (95% CI, 49.5-55.4%).
- N3a (4 or more clinically occult positive lymph nodes with or without in-transit metastases): OS rate 43.2% (95% CI, 39.5-47.2%).
- N3b (4 or more clinically detected positive lymph nodes with or without in-transit metastases): OS rate 36.1% (95% CI 33.1-39.4%).
In contrast, increasing nodal classification groups in the currently used American Joint Committee on Cancer, 8th edition (AJCC-8) system did not strictly correlate with increasing mortality, senior author Zachary Zumsteg, MD, Cedars-Sinai Medical Center, Los Angeles, and colleagues reported in JAMA Surgery.
“{G]iven the heterogeneity of outcomes for patients with node-positive disease, accurate staging and risk stratification is needed to improve patient selection for adjuvant treatment decisions,” Zumsteg and colleagues observed… “we believe that our proposed nodal staging system is generalizable and capable of accurately stratifying patient prognoses across the mortality spectrum.”
According to the study authors, the fundamental issue with the AJCC-8 system is not the variables used but rather the relative weight assigned to them for nodal classification. In contrast, the nodal classification system proposed by Zumsteg et al more accurately stratifies patient prognoses across the mortality spectrum.
“[As such, w]e believe our system should be considered for future versions of cutaneous melanoma staging,” Zumsteg and colleagues wrote.
Patient data for nodal classification development were abstracted from the National Cancer Database, while validation data were abstracted from the Surveillance, Epidemiology, and End Results (SEER-18) database.
In the cohort overall, 59.1% were males with a mean age of 59.9 years.
Just under 17% of patients analyzed had positive lymph nodes, among whom the mean number of metastatic lymph nodes was 2.03. Of these, 22.2% had clinically detected nodal involvement, while the percentage of patients with in-transit disease was very limited at only 1%.
On multivariable analysis, the risk of death was increased by 35% among those with clinically detected metastasis at a hazard ratio (HR) of 1.35 (95% CI 1.27-1.42; P<0.001) while the risk of death for those with in-transit metastasis was 48% higher (HR: 1.48; 95% CI, 1.34-1.65; P<0.001), investigators noted.
“Mortality risk increased sharply with the initial 2 metastatic lymph nodes,” the authors added, more than doubling mortality risk for each positive lymph node (HR: 2.48; 95% CI, 2.37-2.61; P<0.001), after which mortality risk increased more gradually in the presence of 3 or more metastatic lymph nodes (HR: 1.10; 95% CI, 1.07-1.13; P<0.001) for each positive lymph node, they added.
Investigators also validated their proposed nodal classification system in 85,499 patients with cutaneous melanoma identified in the SEER-18 database. Demographics were very similar to those identified in the National Cancer Database.
“Similar to the discovery set, our nodal schema demonstrated continuously increasing overall mortality with increasing nodal classification group,” Zumsteg and colleagues noted. “Cause-specific survival closely mirrored overall mortality rates by nodal classification group in the SEER-18 data set.”
An Improvement Over AJCC-8?
In an editorial accompanying the study, lead editorialist Michael Lowe, MD, Emory University School of Medicine, Atlanta, and colleagues were equivocal about how useful the new classification system might be, suggesting that there were several aspects regarding the applicability of the system that need to be considered.
First, they noted that “[t]he primary outcome used in the proposed model is overall survival compared with the AJCC-8 staging system, which uses melanoma-specific survival.” This means that the cause of death—vital to understanding associations between dependent and independent variables—is often unknown based on analyses of large databases, they argued.
Secondly, Zumsteg and colleagues posited that because completion lymph node dissection (CLND) is no longer compulsory if patients have already undergone sentinel lymph node biopsy, “fewer patients with have high numbers of positive nodes. Thus, some patients who would be assigned a higher N category after CLND likely are assigned a lower stage, potentially affecting risk assessments.”
Inherent biases within both the discovery and the validation databases used to develop the proposed nodal classification system, including inaccurate initial staging, also lend an additional degree of potential confounding to their analysis, they argued.
“Finally, the overall goal of this study was to create a staging system that directly aligns with survival outcomes,” Lowe and colleagues noted. “[H]owever, in doing so, the authors have produced a nodal staging classification that appears less intuitive than the current staging system. By combining elements of pathologic and clinical staging systems and considering the variable treatment of in-transit disease, their model is more complicated. It is not intuitive, for example, that patients with in-transit disease should be grouped with patients with 2 to 3 clinically occult positive lymph nodes. This proposed staging system sacrifices simplicity of classification for simplicity of prognostication. In addition, the proposed model does not identify or clarify any staging strategies that would aid in delineating treatment options.
“The authors should be congratulated on their effort to improve the current staging system [but] we need to ensure that future editions are both accurate and intuitive,” they concluded.
Asked by BreakingMED to comment on the editorial’s critique, Zumsteg in turn agreed with the editorialists’ observation that fewer patients will have high numbers of lymph nodes if they no longer undergo CLND.
“However, the fact that 40% of patients in the database we used did not undergo CLND simply represents real-world practice patterns during the time period of the study and actually represents a strength of the study, not a weakness,” he insisted.
Indeed, because so many patients in the dataset did not undergo CLND, investigators were able to perform a sensitivity analysis where they excluded patients undergoing CLND following sentinel lymph node biopsy to more closely reflect current practice.
“We showed that our system was highly accurate in this subgroup of patients,” Zumsteg explained.
Zumsteg also disagreed with the editorialists’ viewpoint that the proposed nodal classification system is too complex—in fact, he argued that it is simpler than the current AJCC-8 system, which is already quite complex.
“Our system uses the exact same variables as the current system but it has 6 tiers for node positive patients versus 9 tiers in the current system,” he noted—and moreover, he added, as nodal stage increased in the proposed nodal system, the risk of mortality also increased. “What we have done is taken the same variables used in the current system, designed it in such a way that it has fewer groups, more accurately reflects prognosis and produces groups where increasing stage correlates with increasing mortality.”
-
A newly proposed nodal classification system for cutaneous melanoma seemed to accurately predict increasing mortality risk within each nodal classification group.
-
The study authors concluded that their classification system is superior to the standard AJCC-8 system, though experts argued that it is less intuitive and less applicable than the AJCC-8.
Pam Harrison, Contributing Writer, BreakingMED™
The study was supported in part by Cedars-Sinai Cancer.
Zumsteg reported that his spouse performs legal work for Johnson & Johnson and Allergan through her law firm. Coauthors reported relationships with Amgen, Bristol Meyers Squibb, Roche, Genentech, GlaxoSmithKline, and others.
The editorialists had no relevant relationships to disclose.
Cat ID: 105
Topic ID: 75,105,730,105,11,26,192,925,159