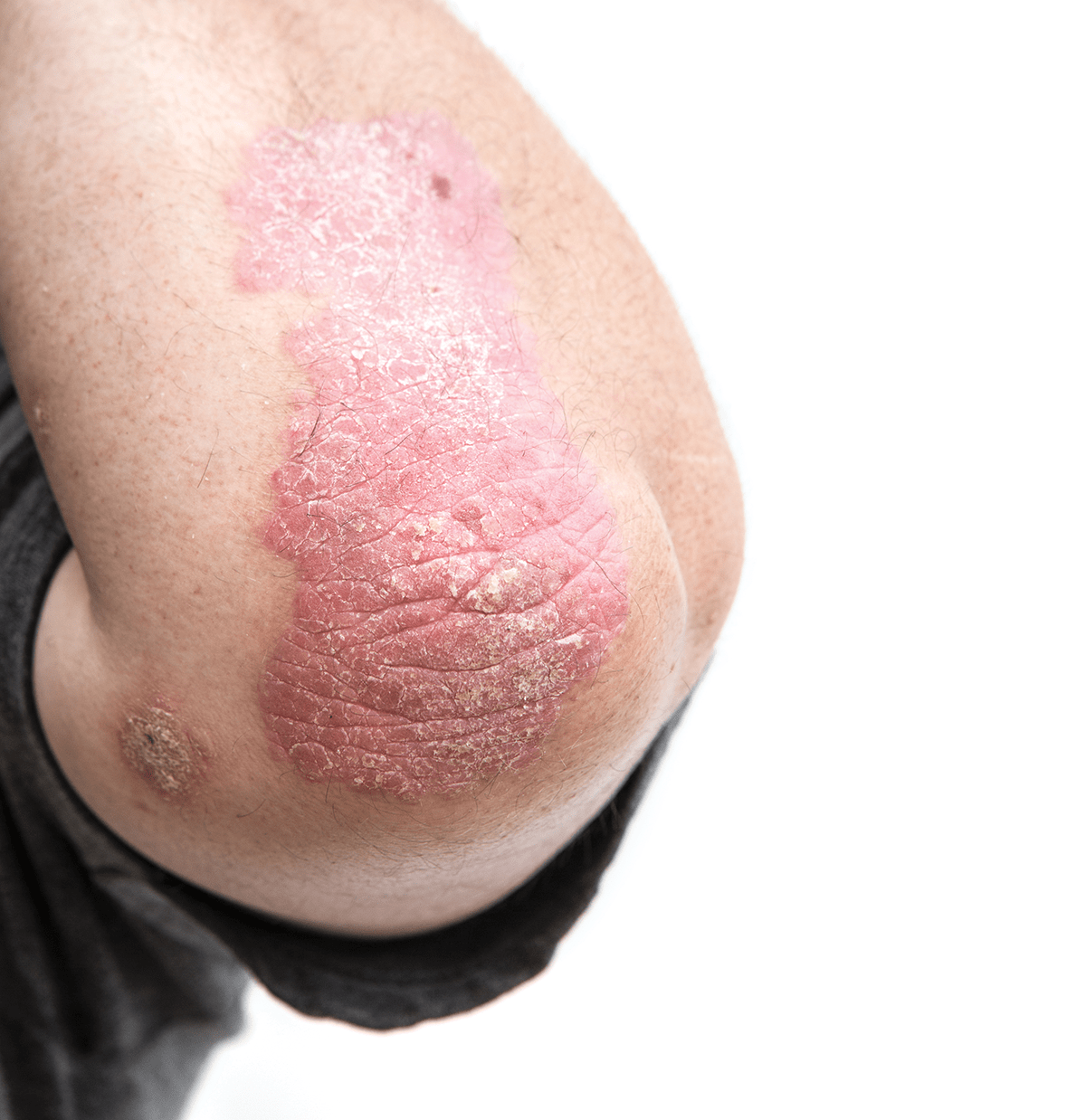
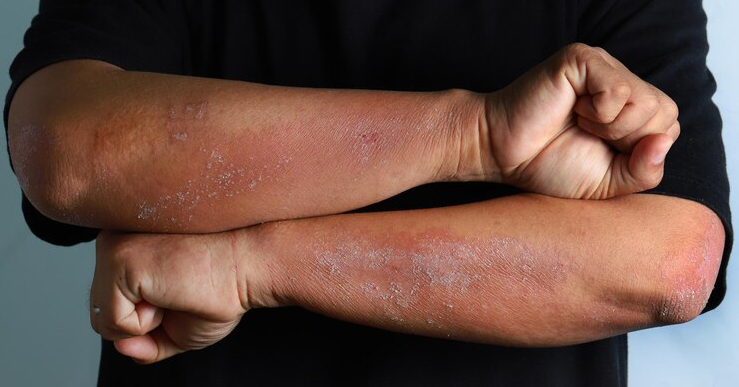
Dermatologists seek simple, reliable assessment tools to make diagnosing psoriasis simpler yet accurate.
Assessment of psoriasis severity is a key component of developing a safe and effective treatment plan. The Psoriasis Area Severity Index (PASI) is considered the gold standard in determining disease severity and is used in myriad clinical trials.
Simpler Assessment Tools Are Needed
According to Wayne Gulliver, MD, although PASI provides valuable insights on the severity of psoriasis in a patient, “most dermatologists do not have the time to perform PASI score on every patient,” he says. Dr. Gulliver and colleagues sought to address this obstacle by examining the efficacy of using body surface area (BSA) and Investigator’s Global Assessment (IGA) to predict results that would otherwise be obtained from PASI and the Dermatology Life Quality Index(DLQI). Dr. Gulliver and colleagues felt that this exploration was important because when compared with PASI and DLQI, “BSA and [Patient Global Assessment] are quick and simple,” he says.
Patients with plaque psoriasis were recruited from 46 US States and Canadian provinces using the CorEvitas Psoriasis Registry, a prospective, multicenter, observational disease-based registry established in 2015 in partnership with the National Psoriasis Foundation. Data from 10,961 patients with plaque psoriasis were included in the study, and these patients participated in 33,605 registry visits that included the collection of PASI and DLQI information at each visit.
PASI Found to Have a Strong Correlation With BSA
The researchers developed a priori 16 linear regression models to calculate predicted PASI and DLQI using a combination of these predictors: BSA, IGA, itch, skin pain, PGA, age, sex, BMI, Modified Charlson Comorbidity Index, and biologic experience. Models were created starting with BSA alone, followed by models adding only IGA, or each patient-reported outcome measure (PROM); this included itch, skin pain, and PGA. Other covariates were also introduced. In addition, prediction models were developed using variable selection methods for the predictors listed above: two linear regressions using stepwise selection procedures via the Akaike information criterion, and one regularized elastic net regression which drew from all conceived variables in addition to interactions of BSA with IGA and PROMs. This resulted in a total of 19 models examined.
PASI was found to have a strong correlation with BSA (r=0.78) and IGA (r=0.66) and was found to have a moderate correlation with DLQI (0.46), PGA (0.44), itch (0.47), and skin pain (0.43). DLQI was moderately correlated with IGA (0.50), PGA (0.57), itch (0.59), skin pain (0.59), and BSA (0.41) (Figure).
In the a-priori-specified models predicting PASI, BSA alone was observed to explain 62% of the variance in PASI (R2adj=0.62; 95% CI, 0.60-0.64). Only slight improvement in predictive abilities was noted when itch, skin pain, and PGA were added to the model (all R2adj=0.64, root mean square error [RMSE] range, 3.32-3.34). The model that paired BSA and IGA performed marginally better compared with the model with BSA alone (R2adj=0.72; RSME, 2.93).
Researchers Are Hopeful About the Future
When asked how the findings of the research team could be incorporated into practice, Dr. Gulliver says that the application of BSA and IGA is “not ready for the clinic yet but [there is] more to come.” Dr. Gulliver is hopeful that the simplicity and ease of use of these alternate assessment methods will aid practicing dermatologists, and that future research focuses on “simple reliable assessment tools” that could make diagnosing and care simpler while remaining accurate.