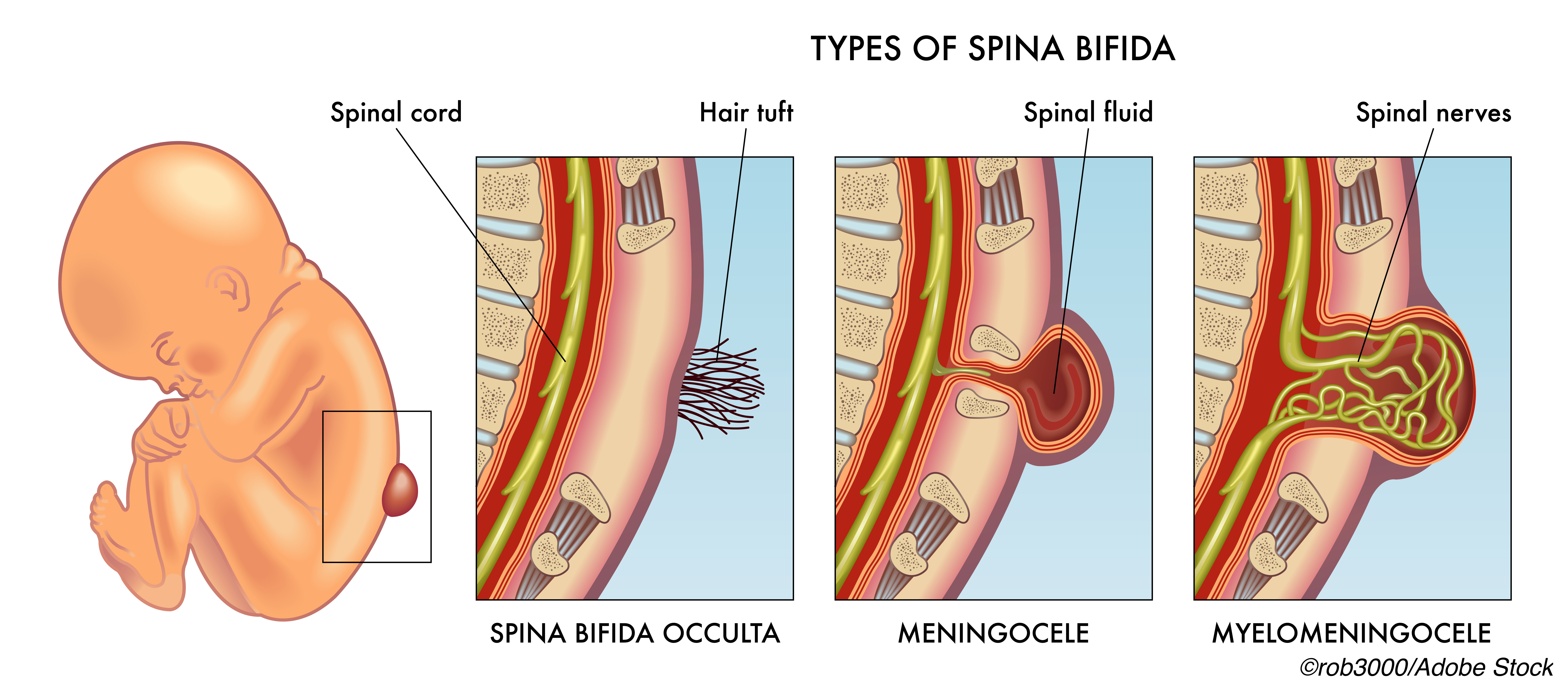
Children with prenatally repaired spina bifida (SB) demonstrated superior performance for self-care, motor function, and mobility versus children who had standard postnatal repair, according to a secondary analysis of the MOMS2 trial.
Among 78 children with postnatal repair and 76 with prenatal repair for myelomeningocele, 96% of the latter group performed age-appropriate self-care skills — chewing and swallowing, using a fork, brushing teeth, doffing pants and socks — compared to the former group at 85.5%, reported Amy J. Houtrow, MD, PhD, MPH, of the University of Pittsburgh Medical Center, and co-authors.
In addition, “Children who underwent prenatal repair had improved motor levels compared with their anatomic levels, walked faster and better with less assistance, and could perform more advanced motor skills,” they wrote in JAMA Pediatrics. “The data presented here demonstrate that the benefits of prenatal repair on mobility persist beyond 30 months.”
This prespecified secondary analysis of MOMS2 delivers “essential new information on long-term outcomes that will affect the prenatal and postnatal management of patients with SB,” wrote Martin Meuli, MD, and Ueli Moehrlen, MD, of from the Zurich-based University Children’s Hospital Zurich, in an editorial accompanying the study.
The data offers “worldwide, first-time evidence that motor spinal levels and, consequently, functional mobility are better in school-aged patients with a history of prenatal rather than postnatal SB surgery…these clinically essential results, durable over a period of 5 to 10 years and thereby persisting into school age, were identified in the very same patients who were, as fetuses, included in the test and control arms of the MOMS trial,” they noted.
Participants in the MOMS trial (2003-2011) were recruited for MOMS2 (2012-2017). The MOMS2 skills testing was conducted by trained examiners, blinded to whether participants were from the prenatal or postnatal intervention group, Houtrow’s group explained. The examiners evaluated the physical characteristics, self-care skills, neurologic function, and mobility, and the investigation was conducted at the same clinical sites as its predecessor or at a child’s home.
Children with postnatal repair had a mean age of 7.4 years and 64.1% were female, while 88.5% were White. Among those with prenatal repair, the mean age was 7.5 years, 56.6% were male, and 92.1% were White.
The last demographic was a study limitation because there was an “underrepresentation of Hispanic children based on the known prevalence of myelomeningocele in the United States,” the authors stated, with previous studies showing that offspring of Hispanic mothers had higher prevalences of SB subtype and most subphenotypes.
Each child underwent assessment for height, arm span, head circumference, and weight, with presence of the following noted: scoliosis, kyphosis, lordosis, leg length discrepancies, varus or valgus knees, foot deformities, contractures at the hip, knee, and ankle, and spasticity.
Functional skills were measured via 34 items selected from the FRESNO scale, and a Modified Hoffer Classification was used to evaluate community ambulators, household ambulators, and non-ambulators. Walk tests were recorded for later analysis, and each child was measured over three attempts.
The authors reported no differences in the percentages of children with spasticity, knee deformities, leg length discrepancies, scoliosis, or kyphosis in either the prenatal or postnatal treatment groups, but foot deformities were another matter. They found that most children in both repair groups had foot deformities, although were fewer contractures in the prenatal surgery group versus the postnatal surgery group:
- Knee: 14.5% versus 36.4%, adjusted relative risk 0.39 (95% CI 0.21-0.72).
- Ankle: 80% versus 92.2%, aRR 0.85 (95% CI 0.75-0.97).
Also, there was no significant difference in the recreational skills category among the groups.
Houtrow and co-authors noted that children in the prenatal repair group were less likely to have a motor function level worse than their anatomic lesion level (aRR 0.44, 95% CI 0.25-0.77), and that the prenatal repair group performed better in the motor category than did the children in the postnatal repair group (93.6% versus 80.5%).
They also found that children in the prenatal repair group were 70% more likely to walk independently in the community (aRR 1.70, 95% CI 1.23-2.34), and to walk without bracing compared with those in the postnatal repair group (32.4% versus 15.3%).
Finally, children with prenatal repair also performed the 10-meter walk test one second faster (1.0 difference in medians, 95% CI 0.3-1.7), had better gait quality (1.71 for adjusted mean difference for home distances of 5 m, 95% CI 1.14-2.54), and could perform higher-level mobility skills (5.70 adjusted mean difference for motor total, 95% CI 1.97-11.18).
Another study limitation was the fact that parents were not blinded to their child’s surgical group, which could have biased their questionnaire responses, the authors noted.
They stressed that “Long-term follow-up of motor skills, ambulatory status, and executive functioning is needed to determine the sustained effects of prenatal repair for myelomeningocele on mobility and functional independence,” while the editorialists said more data were needed on cognition and psychosocial performance over time, as well as the effects of puberty — “patients with SB have a predisposition for pubertas praecox, or abnormally early sexual maturity,” they explained — and a better understanding of to the extent to which “special educational, coaching, and training programs corroborate nonsomatic functions.”
-
Functional mobility and motor levels showed marked improvement for children who underwent prenatal myelomeningocele repair versus standard postnatal repair, according to a secondary analysis of the MOMS2 trial.
-
More than half of the children with spina bifida who underwent prenatal repair could independently walk community distances versus less than a quarter of the children who underwent standard postnatal repair.
Shalmali Pal, Contributing Writer, BreakingMED™
Houtrow reported reported no relationships relevant to the contents of this paper to disclose. A co-author reported support from the NIH and the Eunice Kennedy Shriver National Institute of Child Health and Human Development.
Meuli and Moehrlen reported reported no relationships relevant to the contents of this paper to disclose.
Cat ID: 683
Topic ID: 85,683,730,130,683,192,925,159,161