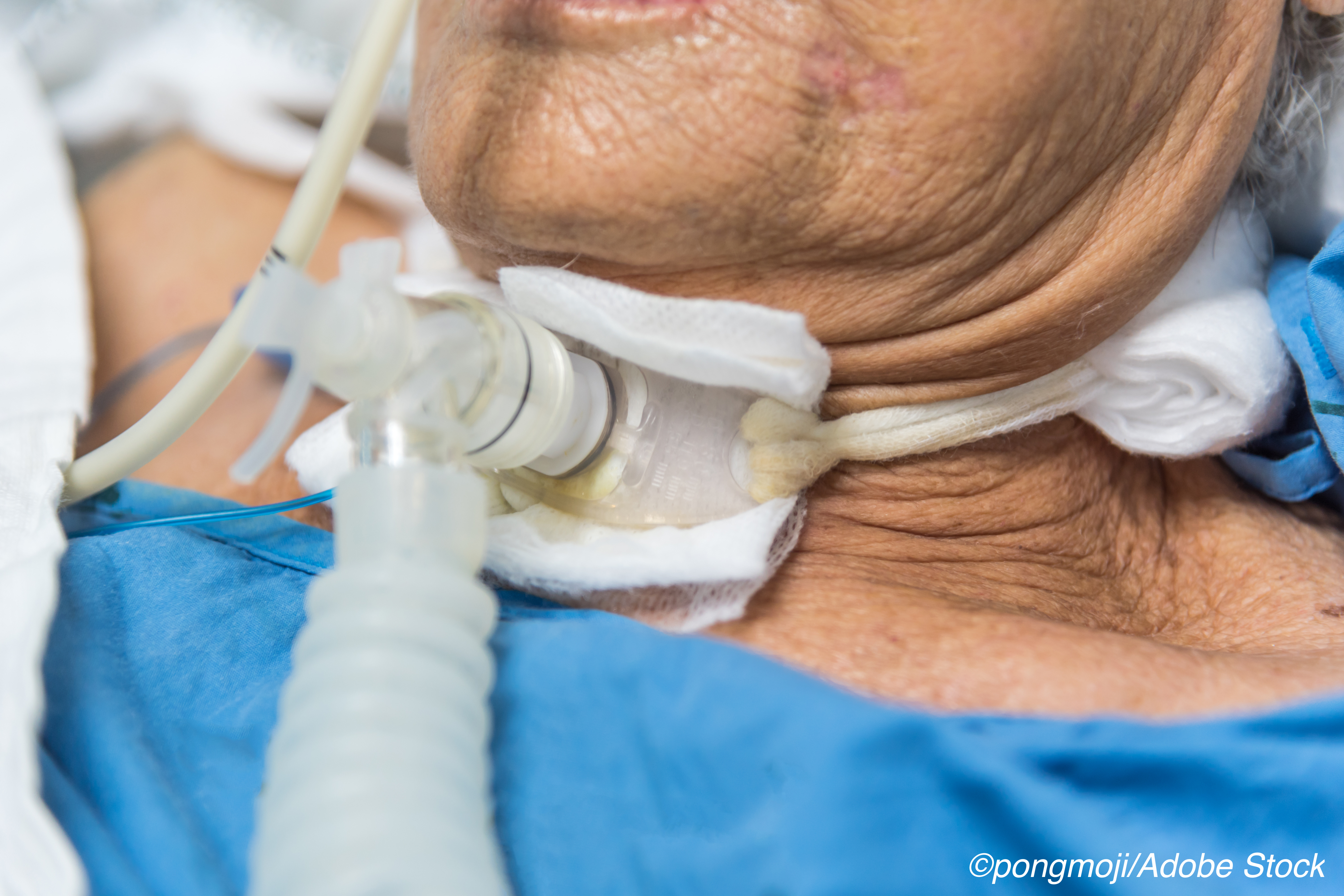
Capping the tracheostomy tube for 24 hours to determine whether a patient is able to breathe on their own is a common practice in tube removal — known medically as decannulation — but protocol-based capping trials may result in removal delays.
The Reducing Decannulation Time Limiting Capping (REDECAP) trial was conducted to compare an alternative assessment strategy based on suctioning frequency to tracheostomy capping for the assessment of decannulation readiness.
Study findings were published online Sept. 9 in the New England Journal of Medicine.
Time to decannulation was 7 days shorter in the airway suctioning-guided group than in the capping group, and these patients also had shorter hospital stays and less pneumonia and tracheobronchitis.
“The most plausible explanation for this result is that capping trials are highly demanding, thus delaying the time to decannulation as reflected by the high proportion of patients with capping trials that failed or of patients with weaning failure,” wrote researcher Gonzalo-Hernandez Martinez, MD, PhD, of Virgen de la Salud University Hospital, Madrid, and colleagues.
The unblinded trial, conducted in five ICUs in Spain, enrolled conscious, critically ill adult patients with tracheostomy tubes who were eligible for enrollment after weaning from mechanical ventilation.
Patients were randomly assigned either to undergo a 24-hour capping trial plus intermittent high-flow oxygen therapy (control group) or to receive continuous high-flow oxygen therapy with suctioning frequency used as the indicator of readiness for decannulation (intervention group).
Specifically, patients in the intervention group underwent decannulation when they had received no more than two aspirations every 8 hours during a 24-hour period, according to prespecified indications.
These indications for suctioning included the presence of rhonchi over the trachea, visible secretions in the airways, an inability to generate an effective spontaneous cough through the cannula despite repeated attempts, suspected aspiration of gastric or upper-airway secretions, acute respiratory distress, or deterioration of oxygen saturation thought to be related to airway obstruction.
The primary outcome was time to decannulation, and secondary outcomes included decannulation failure, weaning failure, respiratory infections, sepsis, multi-organ failure, duration of stay in the ICU and hospital, and death while hospitalized.
A total of 330 patients were included in the trial (mean age 58.3 ± 15.1 years). Just over two-thirds (68.2%) of participants were male and 161 were assigned to the control group and 169 to the intervention group.
Among the main study findings:
- The time to decannulation was shorter in the intervention group than the control group (median, 6 days [interquartile range, 5 to 7] versus 13 days [IQR, 11 to 14]; absolute difference, 7 days (95% CI, 5-9).
- The incidence of pneumonia and tracheobronchitis was lower in the intervention group (4.1% in the intervention group versus 9.9% in the control group; difference, 5.8 percentage points; 95% CI, 0.2-11.8).
- The duration of hospital stay was shorter in the intervention group (mean duration 48 days in the intervention group and 62 days in the control group.
- Decannulation failure occurred in 9 patients (5.6%) in the control group and in 4 (2.4%) in the intervention group (difference, 3.2 percentage points; 95% CI, -1.2 to 8.1).
In an editorial published with the study, critical care specialist Daniela Lamas, MD, of Brigham and Women’s Hospital, Boston, wrote that tracheostomy tubes are needed in approximately 15% of patients who are intubated for respiratory failure and cannot be weaned from ventilator support.
“Decannulation is a key milestone in a patient’s recovery,” she wrote. “But if the procedure is done too soon, a failed decannulation could lead to urgent replacement of the tracheostomy tube or to endotracheal intubation; these are setbacks that involve both physiological and motivational harm,” she wrote.
She noted that there are significant challenges to implementing the decannulation strategy in the United States, including the fact that the procedure is often conducted outside the ICU in post-care facilities. The study population in Spain included only patients receiving ICU care.
“Although the population of patients is reflective of that in the United States, the ratio of nurses and respiratory therapists to patients probably differs, and to obtain broader applicability, these results might be reproduced in a long-term care setting,” she wrote.
She noted that clinical resistance and inertia “in adopting a more aggressive protocol when the standard care does not result in clear harm” represents another challenge to adoption.
But she concluded that “the authors have taken an important step in building an evidence base to improve care for patients with chronic critical illness.”
“The generation of new knowledge should not end when a patient has survived acute illness. As Hernandez Martinez et al. have shown, research in this population is both feasible and necessary.”
-
Patients in ICUs with respiratory failure requiring tracheostomy tubes had shorter time to tube removal when their readiness for removal was based on the frequency of airway suctioning instead of 24-hour capping trial.
-
Time to decannulation was 7 days shorter in the airway suctioning-guided group than in the capping group, and these patients also had shorter hospital stays and less pneumonia and tracheobronchitis.
Salynn Boyles, Contributing Writer, BreakingMED™
Hernandez reported receiving travel support from Fisher and Paykel Healthcare.
Lamas had no disclosures.
Cat ID: 570
Topic ID: 569,570,501,521,728,791,570,573,576,730,192,925


