The following is the summary of “An investigation into the relationship between nutritional status, dietary intake, symptoms and health-related quality of life in children and young people with juvenile idiopathic arthritis: a systematic review and meta-analysis” published in the January 2023 issue of Pediatrics by Zare, et al.
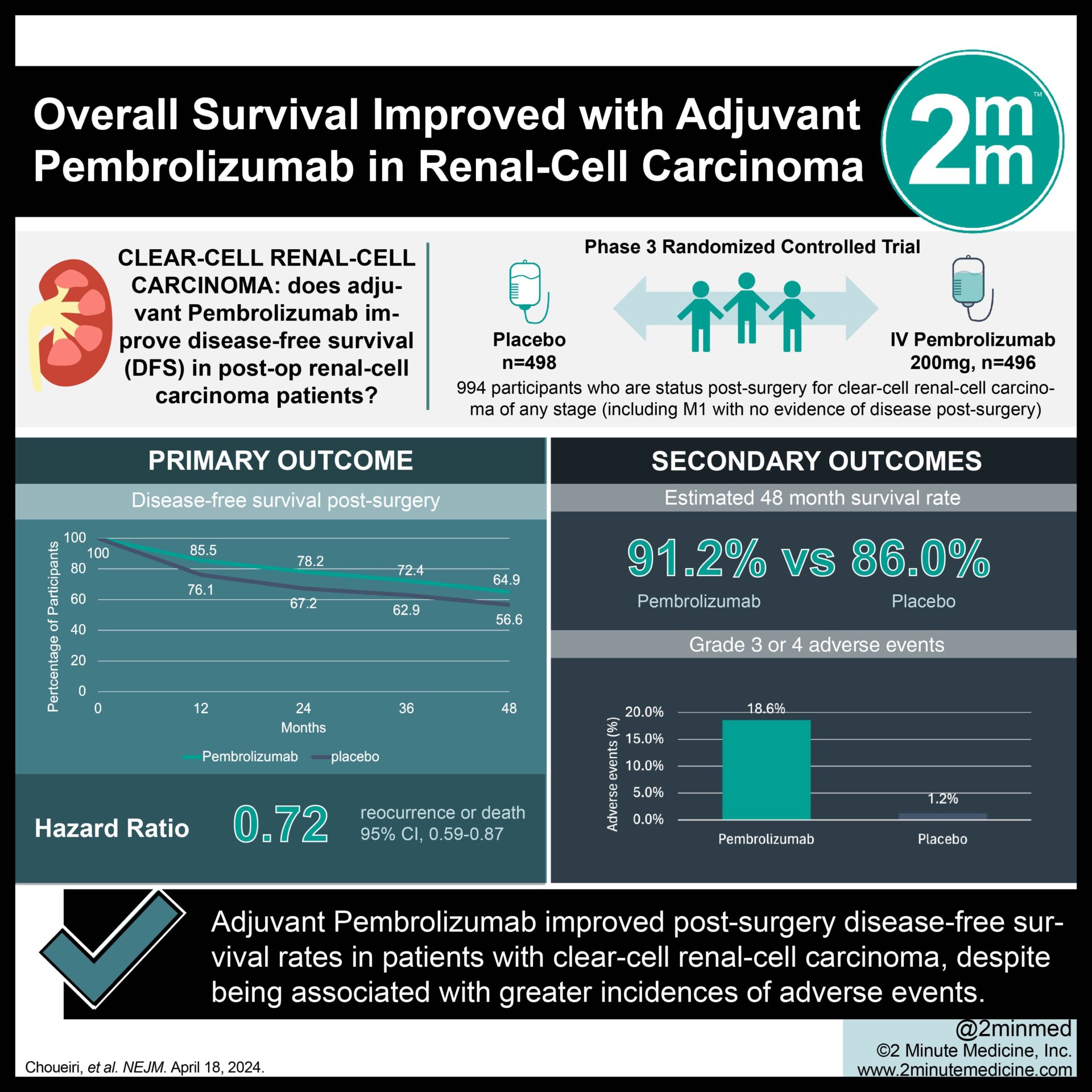
In children and young adults with Juvenile idiopathic arthritis (JIA), the connection between food, symptoms, and health-related quality of life is not well recognized. The purpose of this meta-analysis was to pool data from both observational and interventional studies to draw conclusions on the association between nutritional status, food intake, arthritic symptoms, disease activity, and health-related quality of life in children and young adults with JIA. In October 2019, researchers searched PubMed, CINAHL, PsycINFO, Web of Science, and Cochrane; these databases will be refreshed in September 2020 and October 2021. Only results containing the words “English,” “human,” and “age” were considered (2–18 years old). Quality of life and arthritis symptom management were included criteria for studies examining the impact of diet, vitamin/mineral supplements, or other dietary interventions. They read over the abstracts and titles separately.
Articles that were found to be of interest were obtained in full text. The data extraction process followed the PRISMA recommendations. A random-effects meta-analysis approach was used to compare the effects of 2 independent variables (vitamin D and disease activity). Data were extracted independently by 2 writers using a standardized data extraction form. After scanning the databases, investigators found 11,793 papers; 26 matched our inclusion criteria, including 1,621 participants. The standard of the studies was about average. The average number of active joints (P<0.001), the Juvenile Arthritis Disease Activity Score (JADAS-27) (P<0.001), and immune system (≤ 0.05). All improved with Ɯ-3 PUFA, according to the results of a controlled trial and case control studies, including a total of 146 JIA patients. Furthermore, both n-3 and n-6 PUFAs are inversely related to C-reactive protein(CRP) and erythrocyte sedimentation rate (ESR) (P<0.05). One case study, one pilot trial, and one exploratory study with a total of 9 JIA patients found that Exclusive Enteral Nutrition (EEN), which includes protein and everything else necessary for complete nutrition, reduced JIA symptoms. Clinical research results showed that the Kre-Celazine nutrition program (a unique alkali buffered, creatine monohydrate, and fatty acids combo) reduced JIA symptoms in 16 patients.
About 3 separate investigations all came to the same conclusion: there is no link between vitamin D and illness prevalence. There was a significant (P=0.029) difference between studies in the reported mean height and weight compared to healthy controls. Due to space constraints, study group was only able to incorporate very modest studies (mostly pilots) with a lower-level design hierarchy. They did not find a consistent link between nutrition, symptoms, or health-related quality of life in JIA children and youth, however, they did find evidence of reduced height and weight across studies. The impact of diet on improving symptoms and growth patterns in children and young people with JIA, to improve their quality of life, needs to be determined through well-designed, carefully measured, and controlled interventional studies that take into account important contributing factors like medication and lifestyle behaviors, including physical activity.
Source: bmcpediatr.biomedcentral.com/articles/10.1186/s12887-022-03810-4