The following is a summary of “Ultrasonic Texture Features for Assessing Cardiac Remodeling and Dysfunction,” published in the December 2022 issue of Journal of Cardiology by Hathaway, et al.
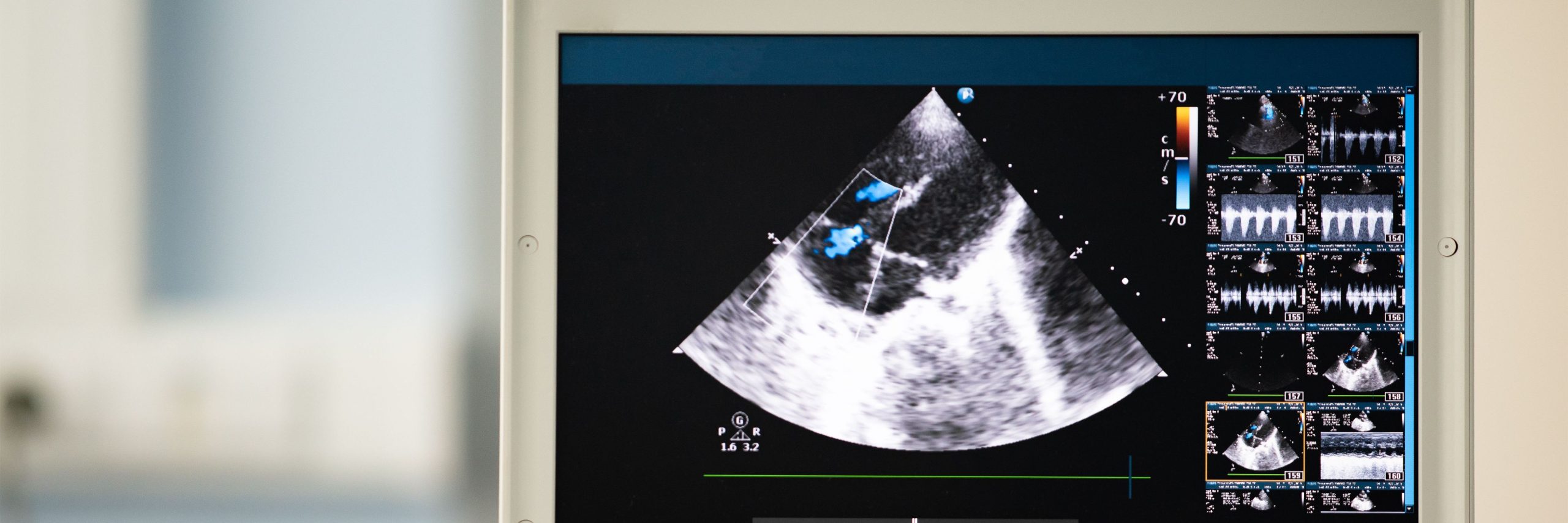
Cardiomyocyte appearance myocardial mass, cardiac size, and eventually, the function of the entire organ is all interconnected characteristics of cardiac remodeling that have a significant impact on patient outcomes. For a study, researchers suggested that using radiomics to extract cardiac ultrasonic textural cues can speed up automated evaluation of left ventricular (LV) shape and function without the need for manual assessments.
In the study, machine-learning models were created using cardiac ultrasound images from 1,915 subjects in 3 clinical cohorts. The cohorts included a prospective POCUS cohort for external validation (n = 275), a prospective external validation on high-end ultrasound systems (n = 484), and an expert-annotated cardiac point-of-care ultrasound (POCUS) registry (n = 943, 80% training/testing and 20% internal validation). The echocardiogram of wild-type (n = 10) and Leptr-/- (n = 8) mice were evaluated longitudinally at 3 and 25 weeks in type 2 diabetic mouse model, and ultrasomics characteristics were linked with histological markers of hypertrophy.
In the external validation trials for POCUS and high-end ultrasound, the ultrasomics model correctly predicted LV remodeling (area under the curve: 0.78 [95% CI: 0.68-0.88] and 0.79 [95% CI: 0.73-0.86], respectively). Additionally, both cohorts’ major adverse cardiovascular events were strongly predicted by the ultrasomics model to be linked with LV remodeling (P < 0.0001 and P = 0.0008, respectively). The ultrasomics likelihood score was also a standalone echocardiographic predictor of major adverse cardiovascular events in the high-end ultrasonography population on multivariate analysis (HR: 8.53; 95% CI: 4.75-32.1; P = 0.0003). Cardiomyocyte hypertrophy and two ultrasomics indicators showed a favorable correlation in the murine model (R2 = 0.57 and 0.52, Q <0.05).
Cardiac ultrasomics-based biomarkers might support the creation of machine-learning algorithms that assess LV shape and function at the expert level.
Reference: jacc.org/doi/10.1016/j.jacc.2022.09.036