The following is a summary of the “Activation of retinal glial cells contributes to the degeneration of ganglion cells in experimental glaucoma,” published in the March 2023 issue of Progress in retinal and eye research by Miao, et al.
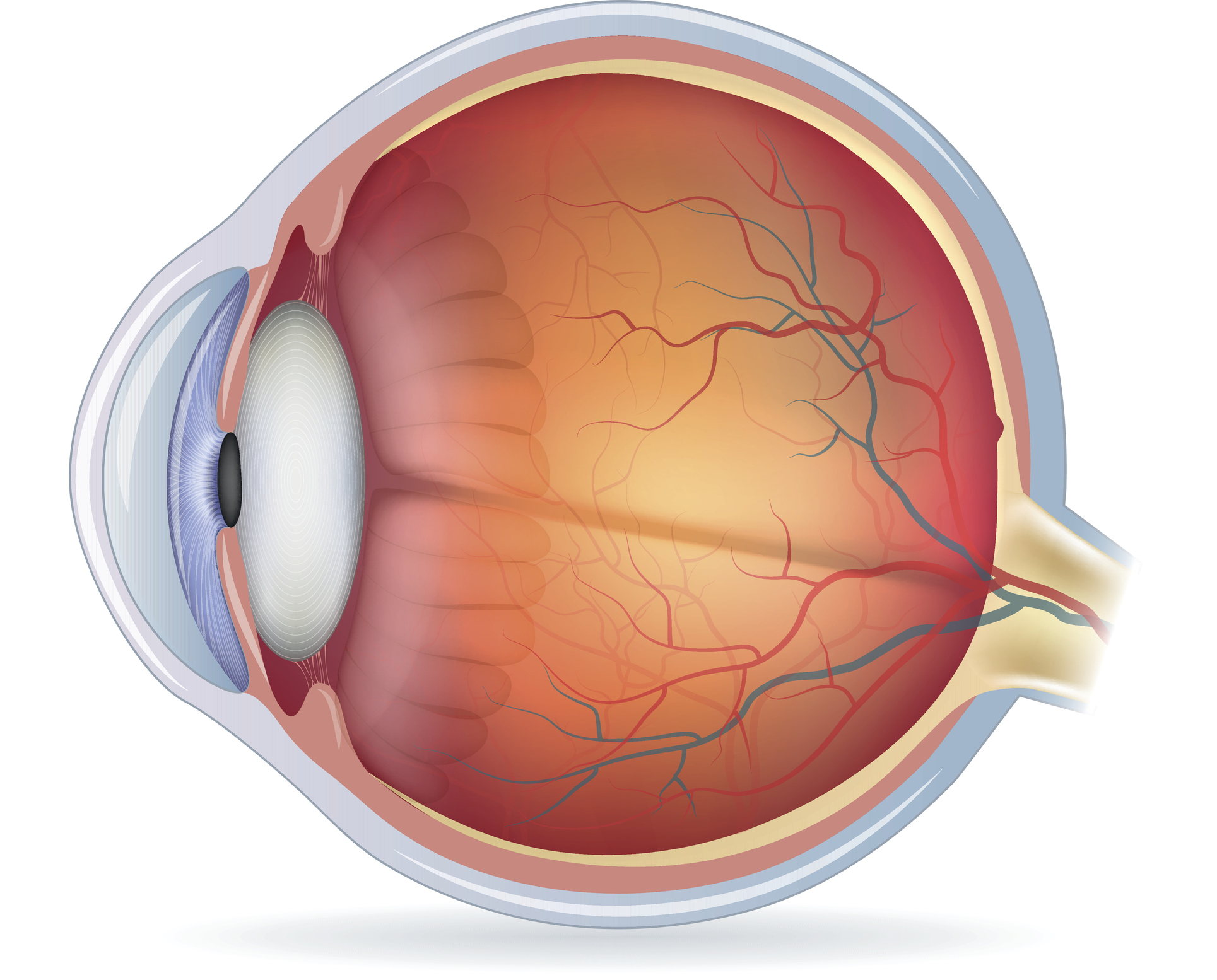
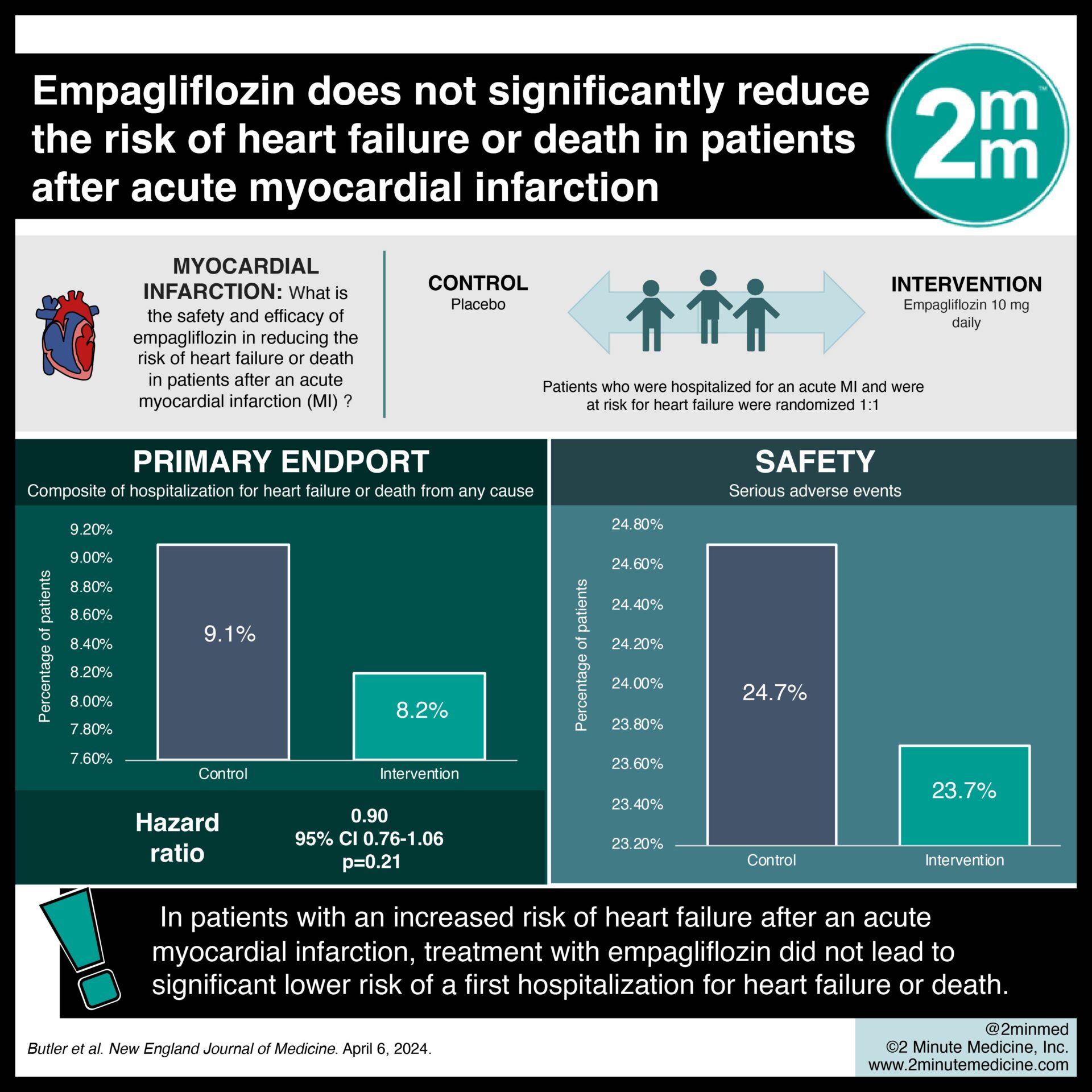
Increased intraocular pressure (IOP) is a major contributor to neurodegeneration in glaucoma. Degeneration of retinal ganglion cells (RGCs) is observed in experimental glaucoma animal models caused by increased IOP, suggesting a significant role for glial cells supporting retinal neurons’ normal function. A rise in IOP triggers the activation of Müller cells by blocking Kir4.1 channels, which in turn activates mGluR I.
After Müller cells become activated, a series of events occur, including proliferation and release of inflammatory and growth factors (gliosis). Several factors regulate gliosis even further. By producing glutamate receptor-mediated excitotoxicity, releasing cytotoxic factors, and activating microglia, activated Müller cells contribute to RGC degeneration. Microglia, resident immune cells in the retina, become activated in response to high IOP, undergoing a series of morphological and functional changes that culminate in adaptive immune responses like the increased release of pro-inflammatory factors (tumor neuronal factor-, interleukins, etc.).
Heat shock proteins, CD200R, chemokine receptors, and metabotropic purinergic receptors further regulate these ATP and Toll-like receptor-mediated responses, which may exacerbate RGC loss. Astrogliosis is initiated and regulated by a complex reaction process involving purines, transmitters, chemokines, growth factors, and cytokines in the optic nerve head, and it releases pro-inflammatory factors. It modifies the extracellular matrix, contributing to RGC axon injury in glaucoma. Glial cell types interact with one another in ways that further modify the effects of activated glial cells on RGCs. The review’s conclusion presents a thorough discussion of future research avenues.
Source: sciencedirect.com/science/article/abs/pii/S1350946223000083