The following is a summary of “Fungal Prosthetic Joint Infection: A Case Series and Review of the Literature, and duration of protection,” published in the April 2024 issue of Infectious Disease by Starnes et al.
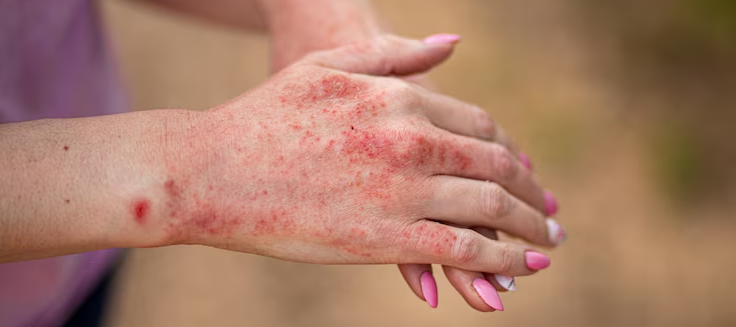
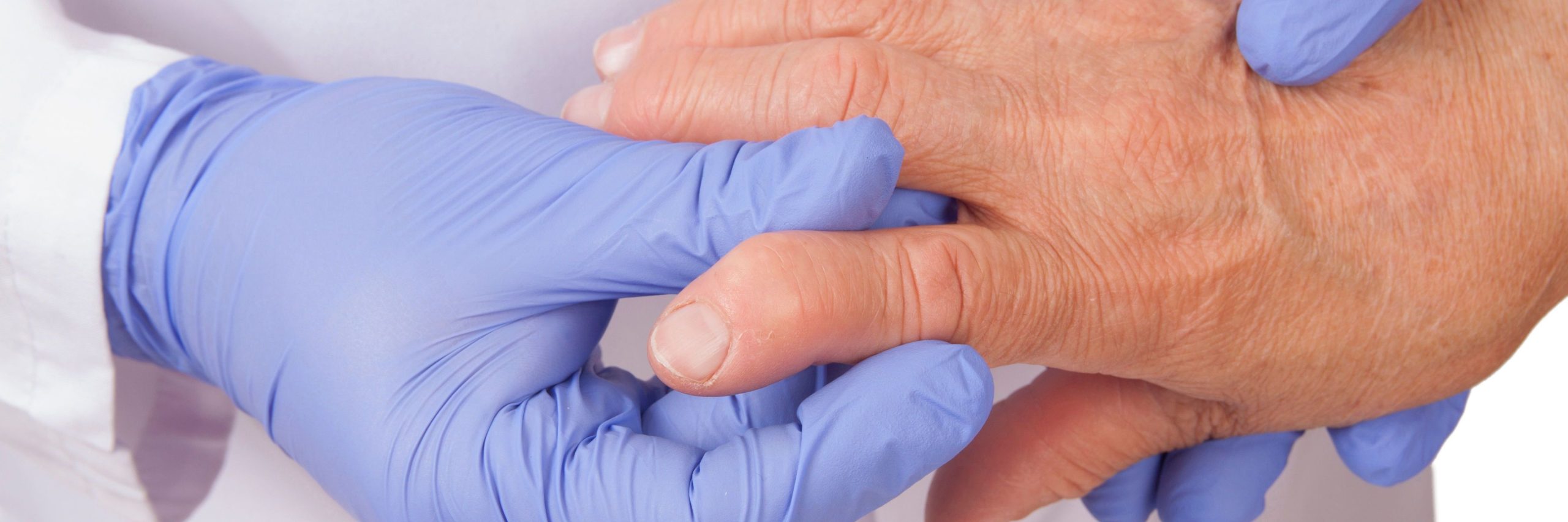
Rare fungal prosthetic joint infections, constituting less than 1% of all such infections, pose a challenge due to limited knowledge about optimal treatment strategies.
Researchers conducted a retrospective analysis to investigate how surgical approach, antifungal treatment, fungal type, and time since initial surgery influence outcomes in patients with rare fungal prosthetic joint infections.
They conducted a retrospective record review spanning 12 years in two health systems, encompassing patients with a deep culture positive for a fungal isolate and a prosthetic joint. They also carried out a literature review with identical inclusion criteria. A total of 289 cases were identified and scrutinized.
The results showed Candida as the predominant isolate, with a two-stage revision being the most frequent surgical approach. The type of surgical intervention demonstrated a statistically significant association with outcome (P=0.022).
Investigators concluded that two-stage revision surgery combined with extended antifungal therapy resulted in superior outcomes for patients with fungal prosthetic joint infections.
Source: link.springer.com/article/10.1007/s40121-024-00964-9