The following is a summary of “Decreasing alloimmunization-specific mortality in sickle cell disease in the United States: Cost-effectiveness of a shared transfusion resource,” published in the January 2024 issue of Hematology by Ito et al.
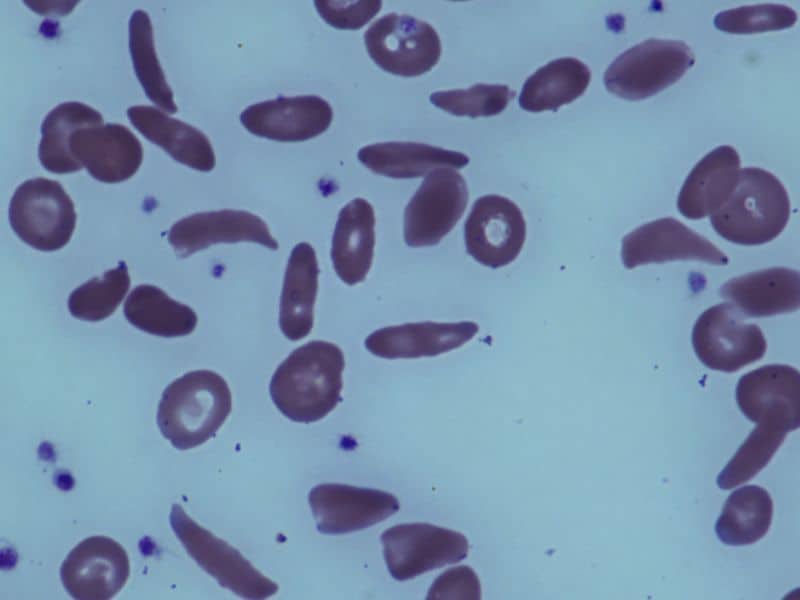
While shared blood resources have lowered delayed hemolytic transfusion reaction (DHTR) and mortality in sickle cell disease (SCD) patients elsewhere, cost concerns in the United States stall similar progress.
Researchers started a retrospective study to estimate how a shared blood resource for alloimmunized SCD patients would affect lifetime DHTR incidence, mortality, quality-adjusted life expectancy (QALE), and costs compared to the current status quo.
They analyzed data over a lifetime and from the perspective of the US health system. Implementation of shared transfusion resource projects reduces cumulative DHTR-specific mortality by 26% for alloimmunized SCD patients in the US compared to the current situation.
The results showed that for 32,000 patients, implementing this intervention would result in a discounted gain of 4,000 QALYs at an incremental cost of $0.3 billion. This yields an incremental cost-effectiveness ratio of $75,600/QALY [95% credible interval $70,200–$81,400/QALY]. Outcomes show sensitivity primarily to baseline lifetime medical expenditure of SCD patients. Alloantibody data exchange proves cost-effective in 100% of 10,000 Monte Carlo simulations. Resource would theoretically need a minimum patient population of 1,819 or an annual cost not exceeding $5.29 million to be considered cost-effective.
Investigators concluded that in the US, simulation suggests a shared transfusion resource for SCD patients would have saved lives and reduced costs through decreased DHTR-specific mortality.