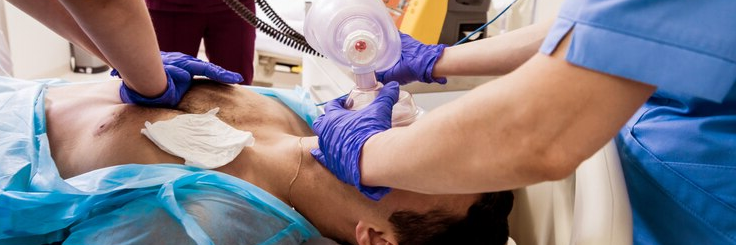
Physicians must remember they took an oath to “do no harm” and must act in accordance with it, even if their choices do not meet a patient’s preferences.
Professionals in all lines of work strive to satisfy their clients, and physicians are no exception. Especially with the growing popularity of online reviews, which are out there for millions of people to peruse in an instant, physicians have a tremendous amount riding on patient feedback. As such, saying “no” to patients when they ask for a certain treatment can be particularly daunting for doctors, even when they are aware that approving the requested treatment or service may not be in the patient’s best interest. Physician and clinical mental health writer Kristen Fuller, MD is all too familiar with such dilemmas.
A few years ago, Dr. Fuller said “no” to a patient who insisted on being treated with antibiotics for a viral infection. Employing patience and thoughtfulness, Dr. Fuller explained to the patient that unnecessary antibiotic use can lead to bacterial resistance, and that plenty of fluids and rest should suffice in overcoming the virus. The patient was uninterested. She had entered Dr. Fuller’s office with a mission—to get a prescription for antibiotics—and she would not be satisfied unless her mission was met. As such, the patient subsequently burned Dr. Fuller with a devastating online review, despite Dr. Fuller’s ethical and empathetic approach.
This incident scarred Dr. Fuller and led her to respond more leniently to some patient requests for fear that saying “no” would generate more scathing online reviews. She began to green-light more treatments and procedures that she believed were medically unnecessary, like pricey imaging tests, diet pills for weight loss, and opioids for mild pain. Nonetheless, Dr. Fuller acknowledges that physicians serve as community leaders, and therefore must learn to stay steadfast and uphold their oath to serve in the best interest of a patient’s health.
According to an article in the January 2018 issue of JAMA Internal Medicine, there is a direct relationship between fulfillment of patient requests and patient satisfaction, and failure to bring patient requests to fruition can put physicians at great risk for poor ratings and reduced compensation. The study authors noted that rejected patient requests were associated with patient satisfaction ratings 10 to 20 percentiles lower than ratings tied to visits in which patient requests were approved.
In an effort to provide optimal support for their patients, physicians often try to work collaboratively with patients when making treatment plans. However, Dr. Fuller notes that physicians must not lose sight of the fact that they took an oath to “do no harm” and must act in accordance with that oath, even if their choices do not meet a patient’s preferences. As such, initiating a dialogue will allow physicians to avoid leaving patients feeling misunderstood or angry. It is important that physicians make a sincere attempt to understand why patients are arguing for or against a particular service or treatment, thereby ensuring that patients feel heard and respected. Patients are, after all, people too. The word “no” can be a bit harsh for anyone, so Dr. Fuller encourages physicians to follow that word with a transparent, empathetic justification acknowledging the patient’s feelings while thoughtfully explaining their medical stance.