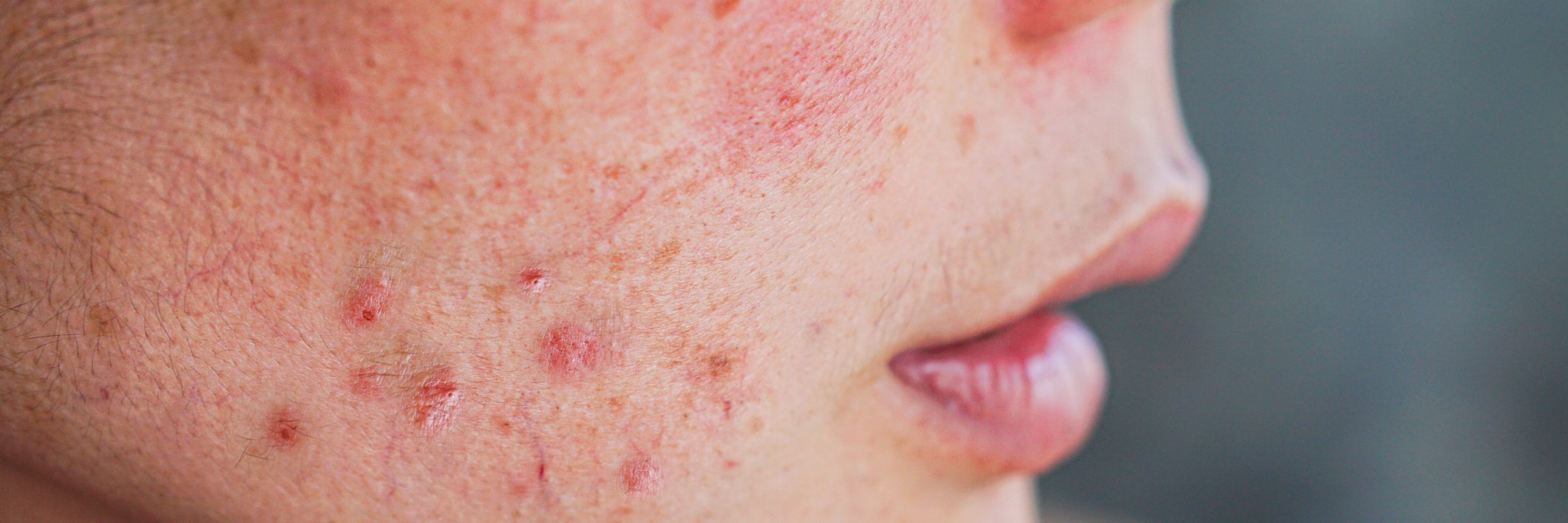
The following is a summary of “Lived Experience of Acne and Acne Treatment in Transgender Patients,” published in the January 2024 issue of Dermatology by Gold, et al.
While acne is prevalent among transgender and gender-diverse individuals and is often linked to gender-affirming hormone therapy, limited research has explored these factors and their effects within gender-minority communities. For a study, researchers sought to investigate the lived experiences of acne and its treatment among transgender and gender-diverse participants.
Conducted from January 4, 2021, to April 7, 2022, this mixed-methods analysis occurred at a multidisciplinary gender center in a public safety-net hospital and endocrinology and dermatology clinics in a tertiary academic center. Participants were transgender or gender-diverse adults who had undergone gender-affirming hormone therapy. Data analysis occurred between November 11, 2021, and March 31, 2023, utilizing semi-structured interviews, surveys, and thematic analysis. Interviews delved into the experience of acne and its treatment, audio recorded, transcribed verbatim, coded using minority stress theory and the socioecological model, and analyzed through thematic analysis. Survey data included gender, self-reported acne severity, impact on skin-specific quality of life, and treatment experiences.
Thirty-two participants (mean age: 32 years; range: 18-57) were included, consisting of 17 transgender men, 11 transgender women, and 4 nonbinary individuals. While 31% rated their skin as clear or almost clear, 34% reported mild acne, and 34% had moderate to severe acne. Participants recounted experiences of rejection and bullying due to acne, leading to social avoidance and negative emotional impacts like depression and anxiety. Acne exacerbated dissatisfaction with body appearance, with transgender women reporting interference with feminine gender expression. Conversely, transgender men sometimes viewed acne positively as a sign of testosterone action. Most participants attempted over-the-counter acne treatments and sought advice from various sources, including physicians, peers, online forums, and social media. Barriers to acne treatment included cost, lack of comprehensive care, mistrust of the healthcare system, and inadequate education on transgender-specific acne care.
The study highlighted the stigma surrounding acne among transgender and gender-diverse individuals and identified barriers to effective acne treatment. Implementing strategies to reduce acne stigma, providing tailored acne care education, facilitating multidisciplinary care, and creating transgender-friendly clinical environments are recommended to mitigate the impact of acne in this population.
Reference: jamanetwork.com/journals/jamadermatology/fullarticle/2813277